Next Lesson - Anatomy and Physiology of the Foregut
Abstract
- The gut tube is a central abdominal structure that is formed by the lateral folding, and has cranial (foregut) and caudal (hindgut) blind end pouches formed by craniocaudal folding. The midgut is the portion between and connects to the yolk sac via the umbilicus.
- The intraembryonic coelom will form the abdominal and chest cavities and is lined by a membrane that will become the peritoneum and pleura.
- Mesenteries are double folds of the peritoneum that suspend organs in the abdominal cavity and communicate blood vessels and other important structures. There are two connecting the gut tube, the dorsal on the ‘back’ and the ventral on the ‘front’. The ventral mesentery only exists until the foregut. This means the cavity is divided into the left (greater) and right (lesser) sacs, but distal to the foregut, there is only the left (greater) sac. The epiploic foramen (Foramen of Winslow) connects the greater and lesser sacs.
- Omenta are sheets of visceral peritoneum. The greater omentum is four layers of peritoneum, and attaches the stomach to the transverse colon. The lesser omentum is made up of only two layers of peritoneum, and attaches the stomach to the liver.
- Some peritoneal organs have no mesentery. They can be primarily retroperitoneal (never had a mesentery, e.g. the kidneys) or secondarily retroperitoneal (did have a mesentery but fused with the posterior abdominal wall, e.g. the ascending and descending colons).
- The foregut extends from the oesophagus to the duodenum proximal to the ampulla of Vater and has a blood supply from the coeliac trunk. During development, the stomach rotates longitudinally and then anteroposteriorly. The lung bud forms from the foregut. The liver and biliary systems develop in the ventral mesentery, and the pancreas develops partially in the ventral and partially in the dorsal mesenteries.
- The midgut stretches from the duodenum distal to the ampulla to the proximal 2/3 of the transverse colon, and is supplied by the superior mesenteric artery. During development, the primary intestinal loop is the rapidly growing intestine that expands out of the abdominal cavity and undergoes a total of 270 degree counter-clockwise rotation. During this rapid growth, the lumen becomes partially occluded, and recanalization restores this.
- The hindgut runs from the distal 1/3 of the transverse colon to the structures of cloacal origin (upper anal canal, bladder). The rectum has two distinct parts with different arterial supplied, lymph drainage, nervous supply and epithelium.
Core
This article covers the development of the gastrointestinal system.
In the fourth week of embryonic development, the trilaminar disc folds in two ways:
First it folds laterally to create a ventral body wall and a tubular primitive gut.
It then folds craniocaudally to form the cranial and caudal blind end pouches from yolk sac endoderm.
The gut tube is an endoderm lined tube that runs the length of the body with blind pouches at the head and tail ends. It opens at the umbilicus via the Vitelline duct.
The foregut and hindgut develop from the head and tail blind pouches, and the midgut develops from the portion that is continuous with the yolk sac (the Vitelline duct).
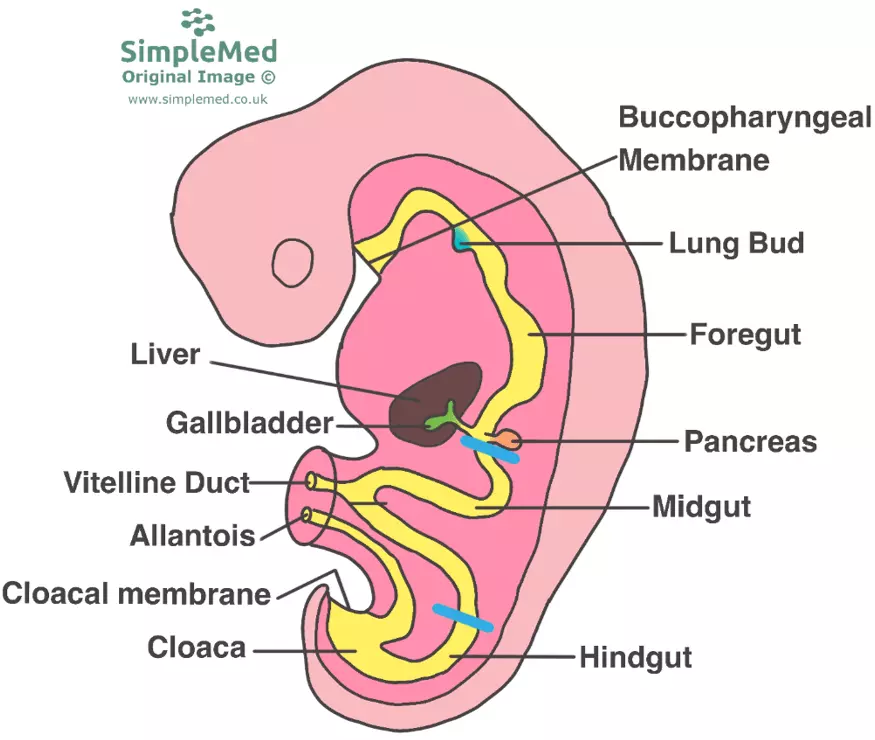
Diagram - The gut tube in the developing embryo. The blind pouches that form the foregut and the hindgut are prevented from being open by the buccopharyngeal and the cloacal membranes
SimpleMed original by Dr. Maddie Swannack
The intraembryonic coelom is a structure that forms from mesoderm during the third week of embryonic development. It is a cavity in the centre of the embryo that, when separated by the developing diaphragm, goes on to form the thoracic and abdominal cavities. One membrane lines the whole intraembryonic coelom, which later specialises, as the cavities do, to form the pleural and peritoneal membranes. A number of key organ systems develop within the coelom.
A mesentery is a double fold of the peritoneal membrane that suspends the gut tube within the intraembryonic coelom away from the abdominal wall. The mesentery allows for gut tube motility and provides a path for the blood and nerve supply from the abdominal wall to the suspended gut tube.
They form from splanchnic mesoderm as a double layer of peritoneum associated with the intraembryonic coelom.
There are two mesenteries attached to the gut tube:
- The dorsal mesentery attaches the ‘back’ of the gut tube to the posterior abdominal wall. It runs the whole length of the gut tube.
- The ventral mesentery attaches the ‘front’ of the gut tube to the anterior abdominal wall. It only attaches the foregut, ending at the distal foregut and leaving a free edge.
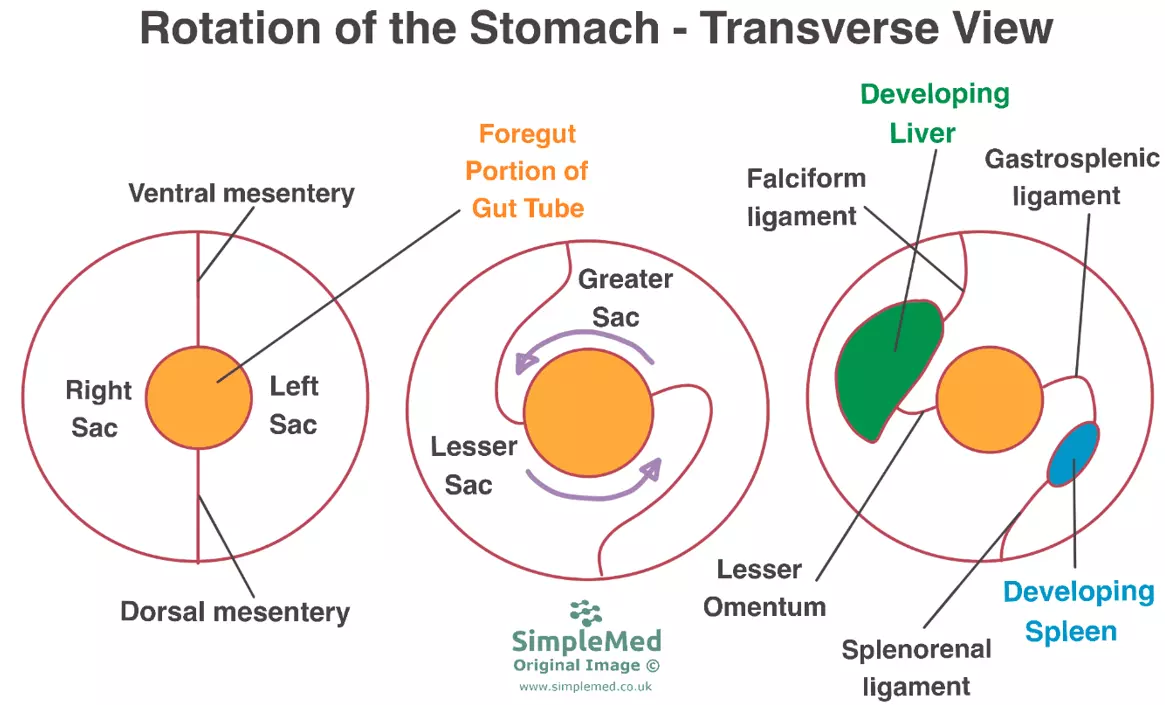
Diagram - The rotation of the foregut. Notice that the gut tube has a dorsal and ventral mesenteries, and the transitions from right sac to lesser sac and from left sac to greater sac. The development of the liver and the spleen are more complex than shown, but it is a good representation of their location
SimpleMed original by Dr. Maddie Swannack
This means that at the foregut, the two mesenteries (dorsal and ventral) divide the cavity (intraembryonic coelom) into two sections, the left and right sacs. Distal to the foregut, however, there is only the dorsal mesentery. This single cavity is the continuation of the left sac.
With further folding and development of the organs, the left sac develops into the greater sac, and the right sac develops into the lesser sac.
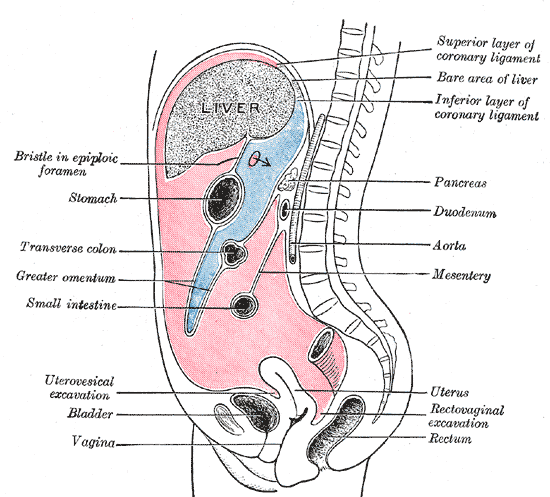
Diagram - The greater sac (in pink) and the lesser sac (in blue) in the sagittal plane. Remember the lesser omentum runs between the liver and the stomach, with the epiploic foramen connecting the greater and lesser sacs. The greater omentum (labelled) is the ‘flap’ with four layers of visceral peritoneum
Public Domain Source Anatomy of the Human Body, by Henry Gray [Public domain]
Omenta are sheets of visceral peritoneum (peritoneum contained within the abdominal cavity covering intraperitoneal organs) extending from the stomach and duodenum to other organs. They form the boundary of the lesser and greater sacs.
The greater omentum is made up of four layers of visceral peritoneum, and attaches to the greater curvature of the stomach and to the transverse colon. It lies like an apron over the front of the intestines in the adult. It has roles in preventing adhesion of organs to the parietal peritoneum and in covering inflamed organs to protect nearby structures which is why it is referred to as the ‘policeman of the abdomen’.
The lesser omentum is made up of only two layers of visceral peritoneum, and attaches to the lesser curvature of the stomach and to the liver. Due to the ventral mesentery ending at the foregut, the lesser omentum has a free edge, which conducts the bile duct, portal vein and hepatic artery to the liver.
The epiploic foramen (foramen of Winslow) is the connection between the lesser and greater sacs.
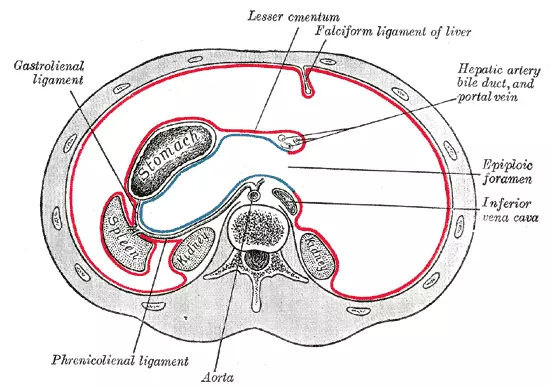
Diagram - The greater (in red) and lesser (in blue) sacs in the transverse plane. It shows the epiploic foramen very clearly
Public Domain Source Anatomy of the Human Body, by Henry Gray [Public domain]
When there is no mesentery, organs are not suspended in the abdominal cavity but are attached to the abdominal wall. This means that they are covered only by parietal peritoneum (the peritoneal layer lining the abdominal wall). These organs can be:
- Primarily Retroperitoneal - these organs were never covered by visceral peritoneum or had a mesentery. These organs developed outside of the abdominal cavity, like the kidneys.
- Secondarily Retroperitoneal - these organs did have a mesentery, but as they grew, the mesentery fused with the posterior abdominal wall, causing the organ to become retroperitoneal. The structure formed by the fusion of the parietal and visceral peritoneum is known as a fusion fascia. Examples of this are the ascending and descending colons.
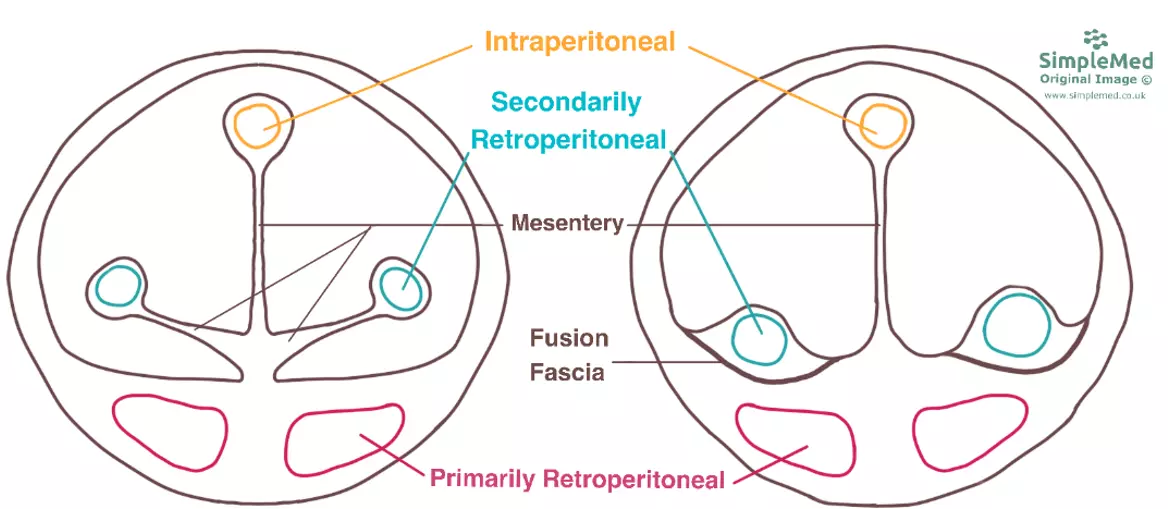
Diagram - The difference between primarily retroperitoneal, secondarily retroperitoneal and intraperitoneal organs. In the image, the abdomen shown on the left is earlier in development than the one on the right
SimpleMed original by Dr. Maddie Swannack
Each organ in the gastrointestinal tract develops from one of either the foregut, midgut or hindgut. Each of these three embryological structures has a singular blood supply, with this artery supplying all of the structures that eventually develop. Each structure also has a specific pattern of visceral nervous innervation which has implications for localisation of visceral pain.
Visceral pain is caused by pathology in visceral organs, often due to stretch, ischaemia or inflammation, and may involve the visceral peritoneum. It is poorly localised, generally referring to the dermatome of the spinal nerve that supplies the pathological organ. If inflammation of the viscera becomes bad enough to irritate the parietal peritoneum, pain is localised much more accurately to over the organ itself as the parietal peritoneum receives somatic innervation.
It is important to remember that some structures that develop on the border between divisions receive their blood supply from both: for example, the duodenum develops from the foregut and the midgut, meaning it receives blood supply from the coeliac trunk and the superior mesenteric artery. This means that duodenal bleeds can be surprisingly severe due to this double blood supply.
The foregut is supplied by the coeliac trunk and the greater splanchnic nerve (T5-9 nerve roots), and so all of the organs that develop from this have blood supply from the coeliac trunk and pain in these organs will localise to the epigastric region (T5-9 dermatomes). Organs that develop from the foregut are:
- Oesophagus
- Stomach
- Pancreas
- Liver
- Gallbladder
- Portion of the duodenum that is proximal to the entrance of the bile duct
The lung bud also develops from an outpouching of the gut tube. See our article on respiratory embryology for more information.
The stomach starts off as a long tube, connected to the abdominal wall by the dorsal and ventral mesenteries. The tube begins by rotating longitudinally (along its long axis). The ventral edge swings around to the right and becomes the lesser curve of the stomach. The dorsal edge swings around to the left and becomes the greater curve of the stomach. When viewed from the ventral (bottom, how a CT scanner would display an image) - the gut tube has gone through a 90 degree rotation anticlockwise.
The curves are of different sizes due to the asymmetrical growth of the stomach. The new greater curve which is lying on the left side grows faster than the lesser curve which is to the right. This process is known as anteroposterior rotation and creates a bulge in the stomach and causes the duodenal end of the stomach tube to be pulled up, creating the classic stomach shape.
The lungs develop from an outpouching of the foregut called the respiratory diverticulum. At around week 4 of development, the tracheoesophageal septum develops, separating the gastrointestinal and respiratory tracts.
Abnormal positioning of this septum can lead to a tracheoesophageal fistula - an abnormal connection between the gastrointestinal and respiratory tracts.
For more information on the development of the lungs, please see the article here.
Development of Other Foregut Structures
The development of the pancreas, liver and duodenum are all linked.
The liver and biliary system develops in the ventral mesentery of the foregut, and the pancreas develops partially in the ventral and partially in the dorsal mesenteries.
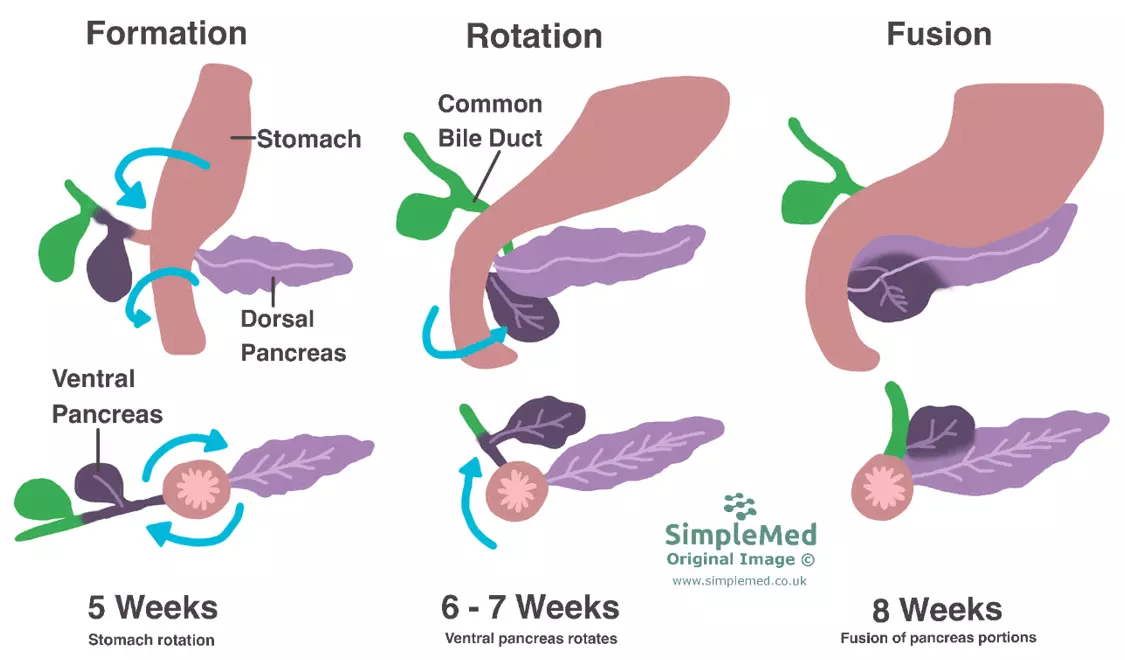
Diagram - The development of the pancreas. It begins in both the ventral and dorsal mesenteries of the foregut, and through rotation and fusion it becomes one gland. This creates the classical ‘C’ shape of the duodenum
SimpleMed original by Dr. Maddie Swannack
The duodenum sits in a ‘C’ shape around the pancreas, pushing the duodenum against the posterior abdominal wall, and causing it to become secondary retroperitoneal.
The midgut is supplied by the superior mesenteric artery (SMA) and lesser splanchnic nerve (T10-11), and so all of the organs that develop from this have blood supply from the SMA and pain in these organs will localise to the periumbilical region (T10-11 dermatomes). Organs that develop from the midgut are:
- Portion of the duodenum that is distal to the entrance of the bile duct (ampulla of Vater)
- Jejunum
- Ileum
- Caecum and appendix
- Ascending colon
- Proximal 2/3 of the transverse colon
The midgut elongates rapidly during development to form the small intestine, however, the abdominal cavity does not grow at the same rate and also contains the rapidly enlarging liver. This means that the growing intestine runs out of space to grow inside the abdominal cavity. As a result it forms a loop that grows outside of the abdominal cavity. This forms a physiological hernia through the umbilicus.
This loop has the superior mesenteric artery as its axis, which supplies blood to the midgut and is connected to the yolk sac by the vitelline duct. The primary intestinal loop can be described as having cranial and caudal limbs divided by the SMA.
Once outside the body, the gut loop makes three ninety degree turns anticlockwise along its axis before returning to inside the abdominal cavity. The turns occur in order to produce a normal adult configuration of organs. As a result of this the cranial limb (more proximal) lies posterior to the caudal limb. This mimics adult anatomy where the more proximal duodenum lies posterior to the transverse colon. The cranial limb ends up on the left side of the abdomen once it has returned into the cavity due to the position of the liver.
Much later in development, the caecal bud descends into the right iliac fossa, forming the classical shape of the intestines in adults.
The growth of the intestine is so rapid that the lumen can become partially or completely occluded. Recanalization is the process of restoring this lumen.
If recanalization is unsuccessful, atresia (complete closure) or stenosis (narrowing) can occur and lead to complications. Failure of recanalization most likely to happen in the duodenum.
It is important to note that failure of recanalization is not implicated in pyloric stenosis. In patients with pyloric stenosis, the lumen develops normally, but hypertrophy of the pyloric sphincter occurs later causing stenosis.
If the gut does not rotate a full 270 degrees anticlockwise or if the loop rotates the wrong way this can lead to an abnormal anatomical configuration. Known as malrotation this condition can increase the risk of volvulus and bowel obstruction in later life. Specific abnormalities include;
- Incomplete Rotation - if only one 90 degree turn occurs, all the colon ends up on the left side, instead of peripherally on all sides.
- Reversed Rotation - if the midgut loop makes one 90 degree turn clockwise, the transverse colon ends up posterior to the duodenum.
There are two key conditions caused by failure for the gut tube to re-enter the abdominal cavity.
- Omphalocele - caused by persisting herniation. The intestine herniates through the abdominal wall but is covered in a layer of peritoneum. Intestinal function may be preserved, but feeding depends on the size of the defect and associated anomalies. It is associated with certain genetic conditions that mean overall it has a worse prognosis than gastroschisis.
- Gastroschisis - caused by failure of abdominal wall closure. The intestine and other organs herniate through the abdominal wall but do not have any peritoneal covering. As a result, they are open to the amniotic fluid and are damaged which will cause issues establishing feeds.
If the vitelline duct which connects the midgut with the yolk sac does not fully obliterate, it can cause various pathologies.
- Vitelline Cysts/Fistulas - a fluid filled remnant of the duct which if open to both the gut and skin forms a fistula.
- Meckel’s Diverticulum - an outpouching of the gut where the duct has not fully obliterated which is not open to the skin and is a blind ending. As it tethers the gut to the abdominal wall it can cause volvulus. It may also contain ectopic glandular tissue which can cause inflammation and pain imitating appendicitis.
- Meckel’s diverticulum is known for its rule of 2’s - 2% prevalence within the population, 2ft from the ileocaecal valve, commonest in under 2y/o, 2:1 male : female prevalence.
The hindgut is supplied by the inferior mesenteric artery (IMA) and lumbar splanchnic nerves (L1-2 nerve roots), and so all of the organs that develop this have blood supply from the IMA and pain in these organs will localise to the suprapubic region (L1-2 dermatomes). Organs that develop from the hindgut are:
- Distal 1/3 of the transverse colon
- Descending colon
- Sigmoid colon
- Rectum
- Structures of cloacal origin:
- Upper 2/3rds of the anal canal (superior to the pectinate line)
- Bladder
- Urethra
The hindgut during development is covered by the cloacal membrane and communicates with the developing genitourinary tract as a structure known as the cloaca. It is an interesting area embryologically as it is one of the few areas where ectoderm meets endoderm without any dividing mesoderm.
Differentiation of the cloaca into the gastrointestinal and genitourinary systems occurs when the urorectal septum descends to divide the two. At this point the cloacal membrane obliterates to form the outlet to the developing bladder and hindgut.
The anal canal is divided into histologically distinct sections by the pectinate line. The pectinate line is the point of demarcation at which the ectoderm and endoderm met during development. The two sections have separate arterial, venous, lymphatic and nervous supplies.
Above the pectinate line, the anal canal is developed from the endoderm. As a result, it is supplied like the rest of the hindgut by the inferior mesenteric artery and the pelvic splanchnic nerves. The sphincters also have parasympathetic innervation by nerves of roots S2, S3 and S4. It is lined with columnar epithelium and is drained by the internal iliac lymph nodes. This means that only stretch can be sensed in this region, a visceral sensation.
Below the pectinate line, the anal canal is developed from the ectoderm. As a result of this differing embryological origin it has a separate neurovascular supply and lymphatics. The canal at this point is supplied by the pudendal artery and the pudendal nerve (spinal nerve root S2, S3 and S4). As this area is ectoderm derived, somatic sensations of temperature, touch and pain can be detected. It is lined with stratified epithelium and drains to the superficial inguinal lymph nodes.
If there are issues in septation of the cloaca or rupture of the membrane this can cause abnormalities in the adult anatomy.
- Imperforate Anus - the cloacal membrane does not rupture and so persists meaning there is no outlet from the gastrointestinal tract and therefore no anus. This will need surgical fixation.
- Fistulae - if there are holes in the septum there can be abnormal connections between the anus and the bladder as they are not properly separated in development.
- Anorectal Agenesis - a severe defect where there is no development of the anus or rectum rather than simply no outlet.
Edited by: Dr. Ben Appleby
Reviewed by: Dr. Thomas Burnell
- 15215

