Next Lesson - Conditions of the Lower Back
Core
Want more information on anatomy before you begin looking at conditions? Head to our articles on Bones of the Lower Limb and Muscles of the Thigh for more information!
The neck of the femur connects the head of the femur to the shaft. Neck of femur fractures can be divided into two categories - intracapsular and extracapsular.
Intracapsular fractures are more common in women and the elderly (those with osteoporosis, which is most common in these demographics). They present with a shortened, adducted and externally rotated leg at the hip.
The medial femoral circumflex artery is at risk of injury (this risk is increased if the fracture is displaced) and damage to this artery can cause avascular necrosis to the femoral head, as it is the main artery that supplies the head of the femur. As a result, it is vital that the blood supply is restored quickly, to prevent permanent damage to the femoral head. Treatment often involves a full or partial hip replacement especially in the elderly.
Extracapsular fractures are more common in young/middle-aged people. They also present with a shortened, abducted and externally rotated leg at the hip due to the distal fragment being pulled upwards and rotated laterally. Avascular necrosis is very rare in extracapsular fractures because the fracture is distal to the medial femoral circumflex artery, so the blood supply remains intact.
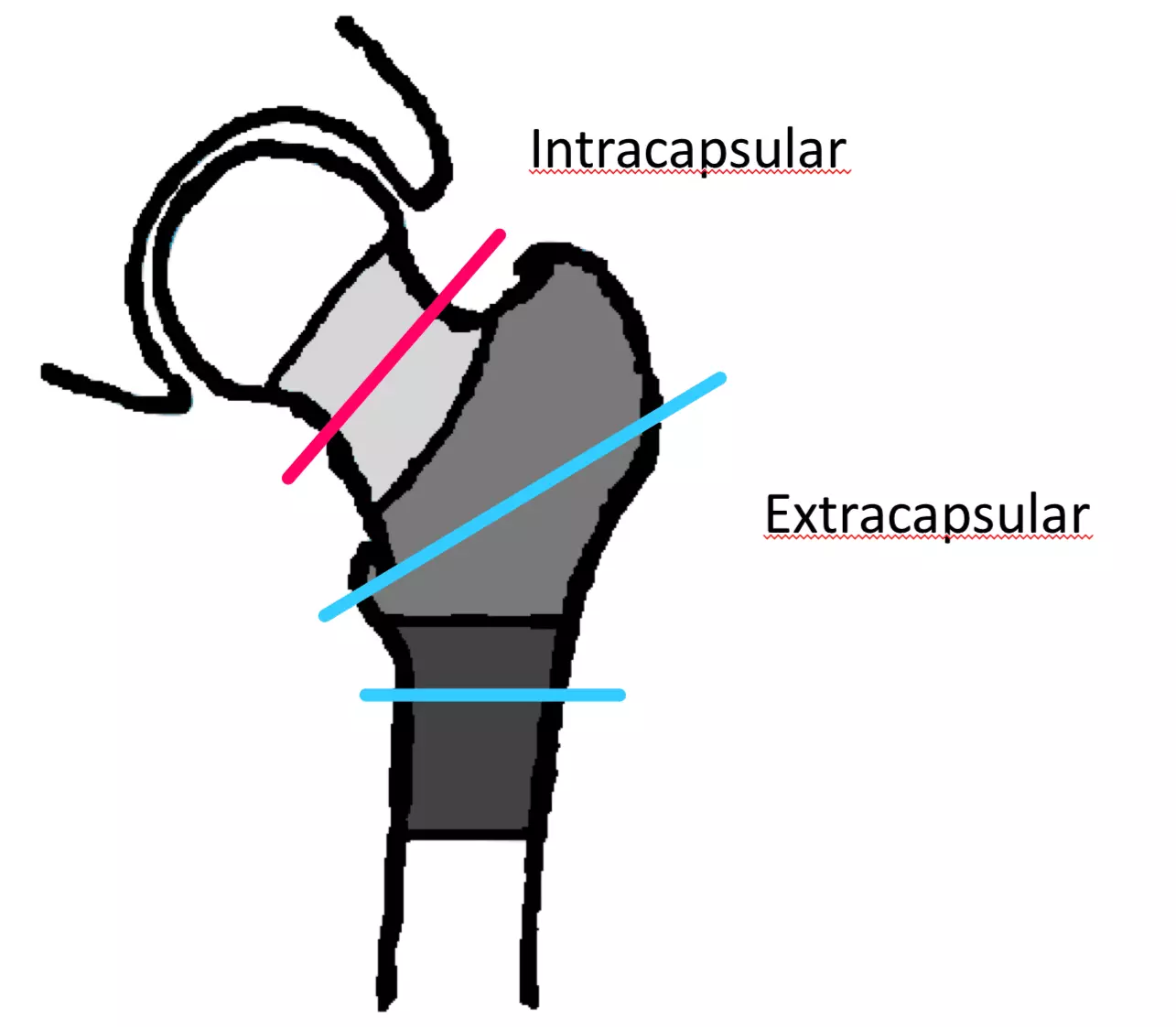
Diagram - The two main types of femoral neck fractures
Creative commons source by Doctodoc, edited by Dr. Laura Hansell [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)]
Hip dislocation occurs when the femoral head is no longer in contact with the acetabulum of the pelvic and can be divided into two categories - anterior and posterior. The hip joint is a stable joint, with many ligaments to support it, meaning that any dislocation needs to have significant force behind it.
90% of all hip dislocations are posterior (femoral head is posterior to where it should be) and are most commonly caused by injuries similar to the knee impacting on the dashboard in a car accident. They present with a flexed, adducted and internally rotated leg at the hip. Posterior dislocations are often associated with sciatic nerve palsy, which has a significant impact on the motor function of the limb.
Anterior dislocations are much less common and the mechanism of injury is usually linked to skiing. They present with a flexed, abducted and externally rotated leg at the hip. A femoral nerve palsy may also be present, but this is relatively uncommon.
Treatment in both cases is hip reduction (significant analgesia required) followed by rehabilitation.
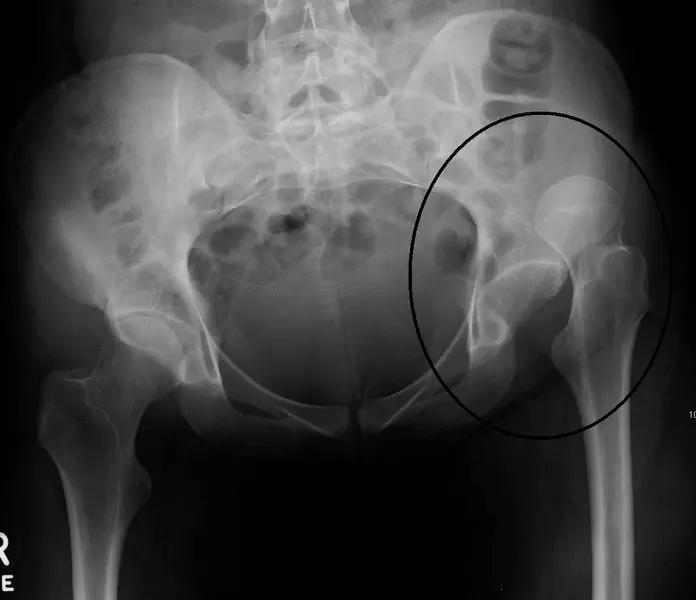
Image - An X-ray of a superior hip dislocation
Creative commons source by James Heilman, MD [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)]
Osteoarthritis (OA) of the hip becomes more common with increasing age and is a frequent cause of pain and disability in older adults. It usually presents with joint stiffness, mechanical pain in the hip, gluteal and groin regions that radiates to the knee, and reduced mobility. The primary cause of OA is unknown, but it can occur secondarily to trauma, infection, rheumatoid arthritis and metabolic disorders.
First line treatment for OA of the hip is over the counter painkillers and lifestyle changes to increase fitness and lose weight. Eventually, a hip replacement may be needed.
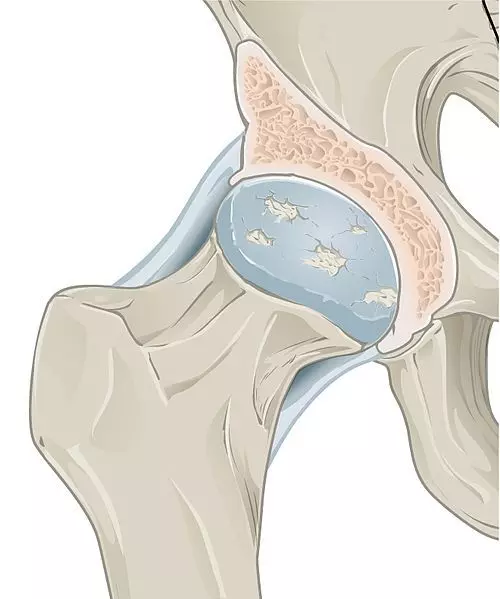
Image - Osteoarthritis affecting the hip joint
Creative commons source by CFCF [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)]
Injury to the Superior Gluteal Nerve
Damage to the superior gluteal nerve typically presents with Trendelenburg’s sign - dropping of the pelvis on the contralateral side to the nerve injury when standing on the leg of the affected side. This occurs as the superior gluteal nerve supplies gluteus medius and gluteus minimus, and the function of these muscles is to stabilise the hip. The patient may use their trunk muscles to compensate when walking, causing them to lean to one side; this is called Trendelenburg gait.
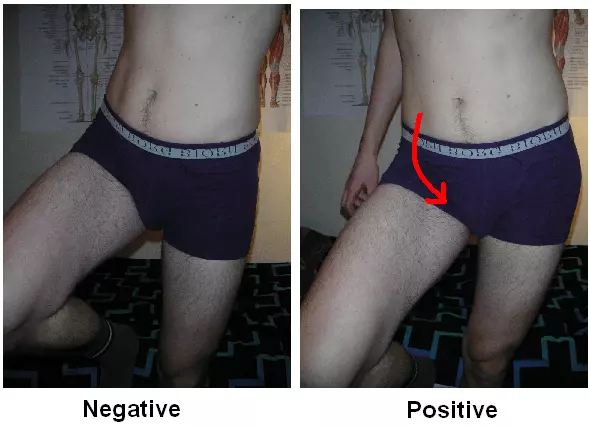
Diagram - A positive and a negative Trendelenburg's sign
Creative commons source by Mikael Häggström [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)]
Reviewed by: Dr. Thomas Burnell
Edited by: Dr. Maddie Swannack
- 6936

