Next Lesson - Structure of Bones
Abstract
- Connective tissue provides support, transportation, protection, storage, defence against infection and aids in wound healing in many tissues around the body.
- Connective tissue contains many types of cells, primarily fibroblasts, which synthesise the extracellular matrix, collagen and ground substance, producing the structural framework of connective tissue.
- They also contain a number of fibre types, dependent on function, such as collagen, reticular and elastic.
- All of these are embedded in ground substance, which is a viscous, slippery substance with a high water content, composed primarily of proteoglycans.
- Connective tissue can be described as loose or dense. Dense can further be divided into regular and irregular dense connective tissue.
Core
The simplest way of understanding connective tissue is to take a complex definition and break it down bit-by-bit.
"a tissue of mesodermal origin that consists of various cells (such as fibroblasts and macrophages) and interlacing protein fibres embedded in a chiefly carbohydrate ground substance, that supports, ensheathes, and binds together other tissues, and that includes loose and dense forms (such as adipose tissue, tendons, ligaments, and aponeuroses) and specialised forms (such as cartilage and bone)."
Let's break it down:
"A tissue of mesodermal origin" -
This simply means a specialised collection of cells which, in the gastrulation stage of fetal development, was developed from the mesoderm layer (there are three germ layers, the other two layers are the ectoderm (outside layer) and endoderm (inside layer), with the mesoderm as the middle layer between them).
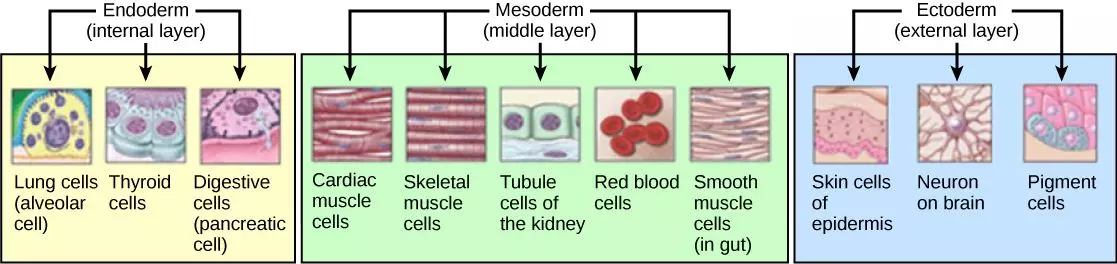
Figure: The germ layers present during the gastrulation stage of fetal development and what develops from each. Connective tissue structures develop from the mesoderm.
Creative Commons Source CNX [CC BY-SA 3.0 (https://creativecommons.org/licenses/by-sa/3.0)]
"that consists of various cells (such as fibroblasts and macrophages)" -
The cells present in connective tissue are:
Fixed cells - do not move within the tissue:
- Fibroblasts - the most common cell in connective tissue, their role is to synthesise the extracellular matrix, collagen and ground substance, producing the structural framework of connective tissue.
- Other cells: Melanocytes (produce the pigment within the skin), Mast cells (granulocyte-containing immune cells), Macrophages (professional phagocytic antigen presenting cells), Adipocytes and Mesenchymal stem cells.
Wandering cells - able to exit and enter tissues, these are immune cells that monitor the tissues for infection:
- Leucocytes, plasma cells, monocytes, eosinophils, basophils.
"and interlacing protein fibres" -
The fibres present in connective tissue are:
These are flexible and have a high tensile strength - the most common protein in the body, 90% of which is "type 1" collagen (of 28 types). Type 1 collagen's structure is that of a triple helix of alpha chains as seen below:
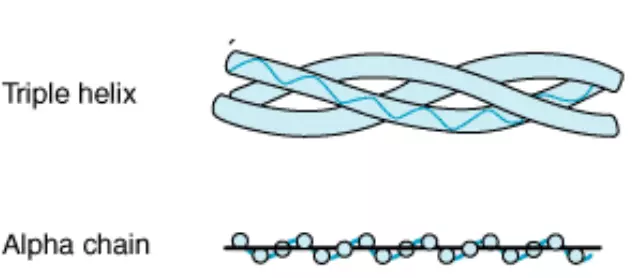
Figure: The structure of collagen, formed from a triple helix of alpha chains.
Fibroblasts secrete procollagen, which is then converted to collagen molecules outside the cell and aggregated to form the final collagen fibrils. Vitamin C is essential for the hydroxylation of proline and lysine residues in procollagen, which is crucial for stable collagen formation. A deficiency in vitamin C can lead to scurvy, characterized by poor wound healing and impaired bone formation. Abnormality in type 1 collagen production can also cause Osteogenesis Imperfecta.
Reticular fibres are a type of fibre composed of type III collagen secreted by reticular cells. Reticular fibres are able to cross-link to form reticulin - this network acts as a supporting mesh in soft tissues such as liver, bone marrow, and the tissues and organs of the lymphatic system.
Elastic fibres allow tissues to recoil after stretch or distension. Elastin is the primary component of elastic fibres, where it is surrounded by microfibrils called fibrillin. It occurs in most connective tissues but to varying degrees. Elastic fibres are particularly important in the artery walls and dermis. Marfan's syndrome is an autosomal dominant disorder in which expression of the fibrillin gene is abnormal, making the elastic tissue abnormal. Sufferers are abnormally tall, exhibit arachnodactyly, have frequent joint dislocation and can be at risk of catastrophic aortic rupture.
"embedded in a chiefly carbohydrate ground substance" -
Ground substance is a viscous, slippery substance with a high water content, composed primarily of proteoglycans.
Proteoglycans are a large macromolecule consisting of a core protein, with glycosaminoglycans (GAGs) attached. These GAGs attract water and form a gel that permits diffusion but resists compression.
Hyaluronic acid is a unique GAG that forms very large proteoglycan aggregates by binding to proteoglycans (such as aggrecan) via link proteins. These highly hydrophilic complexes help cartilage resist compression while remaining flexible. In cartilage, the main GAGs within proteoglycans are chondroitin sulfate and keratan sulfate.
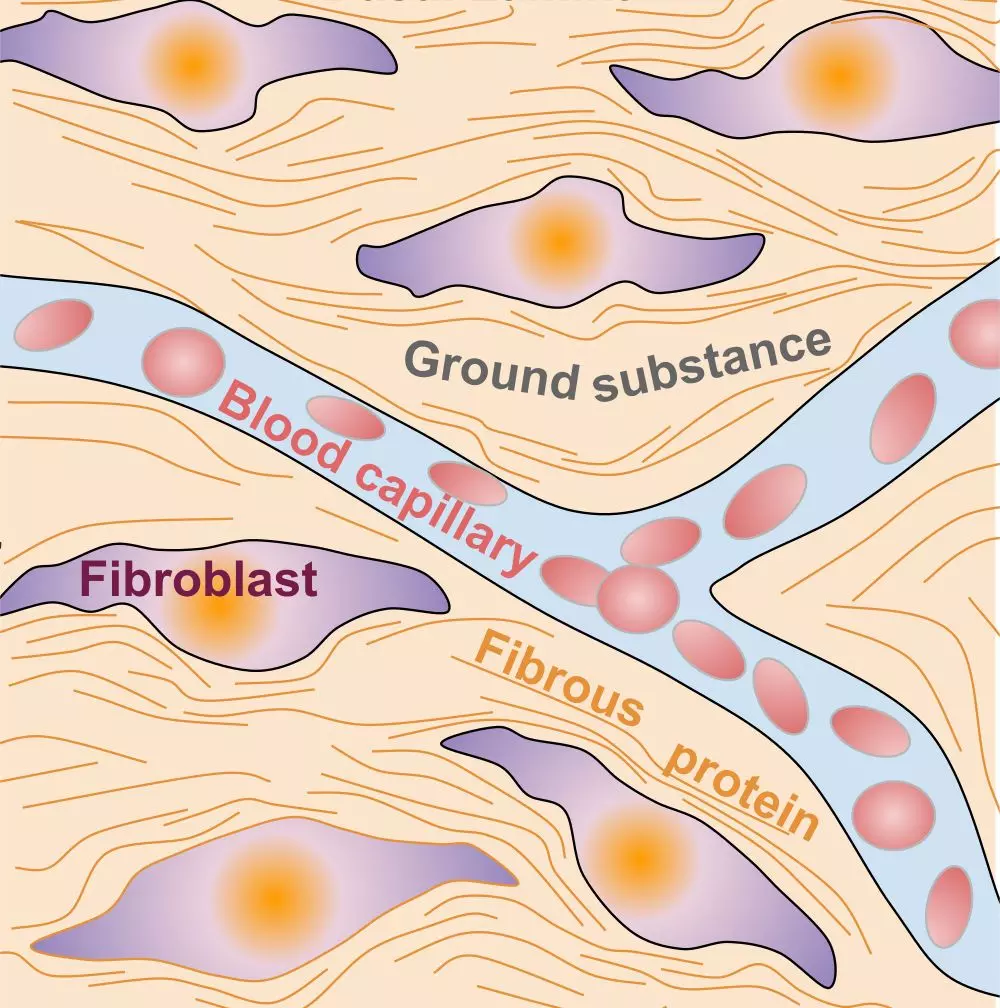
Image: Shows the arrangement of fibroblasts within an extracellular matrix of fibrous proteins and ground substance.
Creative Commons Source Sagearbor [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)] modified by Dr. Marcus Judge
"that supports, ensheathes, and binds together other tissues" -
There are a number of roles of connective tissues - here are the 6 key ones:
- Connects cells to form tissues, connects tissues to form organs and connects organs to form the body.
- Transportation - as they provide a medium through which diffusion of nutrients can occur.
- Protection - provides a cushion between tissues.
- Storage - in the case of adipose tissue, a type of connective tissue.
- Defence against infection
- Wound healing
"and that includes loose and dense forms (such as adipose tissue, tendons, ligaments, and aponeuroses) and specialised forms (such as cartilage and bone)" -
Connective tissue can be:
Loose - contains many cells, few collagen fibres, much ground substance and has a viscous consistency. Loose connective tissue is primarily located directly beneath the epithelia and around blood vessels, areas where bacteria or viruses which have breached the epithelial surface can be attacked and destroyed by the large number of immune cells present in the highly viscous loose connective tissue.
Dense - contains few cells, almost all of which will be fibroblasts (for fibre formation), many collagen fibres and little ground substance. Dense connective tissue can be further split into:
- Regular dense - Collagen fibres are arranged in parallel bundles and are densely packed. Between the bundles are fibroblasts - Designed to withstand stress in a single direction - Seen in tendons, ligaments and aponeuroses.
- Irregular dense - Collagen fibres are arranged in bundles orientated in various directions. Between the bundles are fibroblasts - Designed to withstand stress in multiple directions - Seen in the submucosa of intestine and deep layers of dermis.
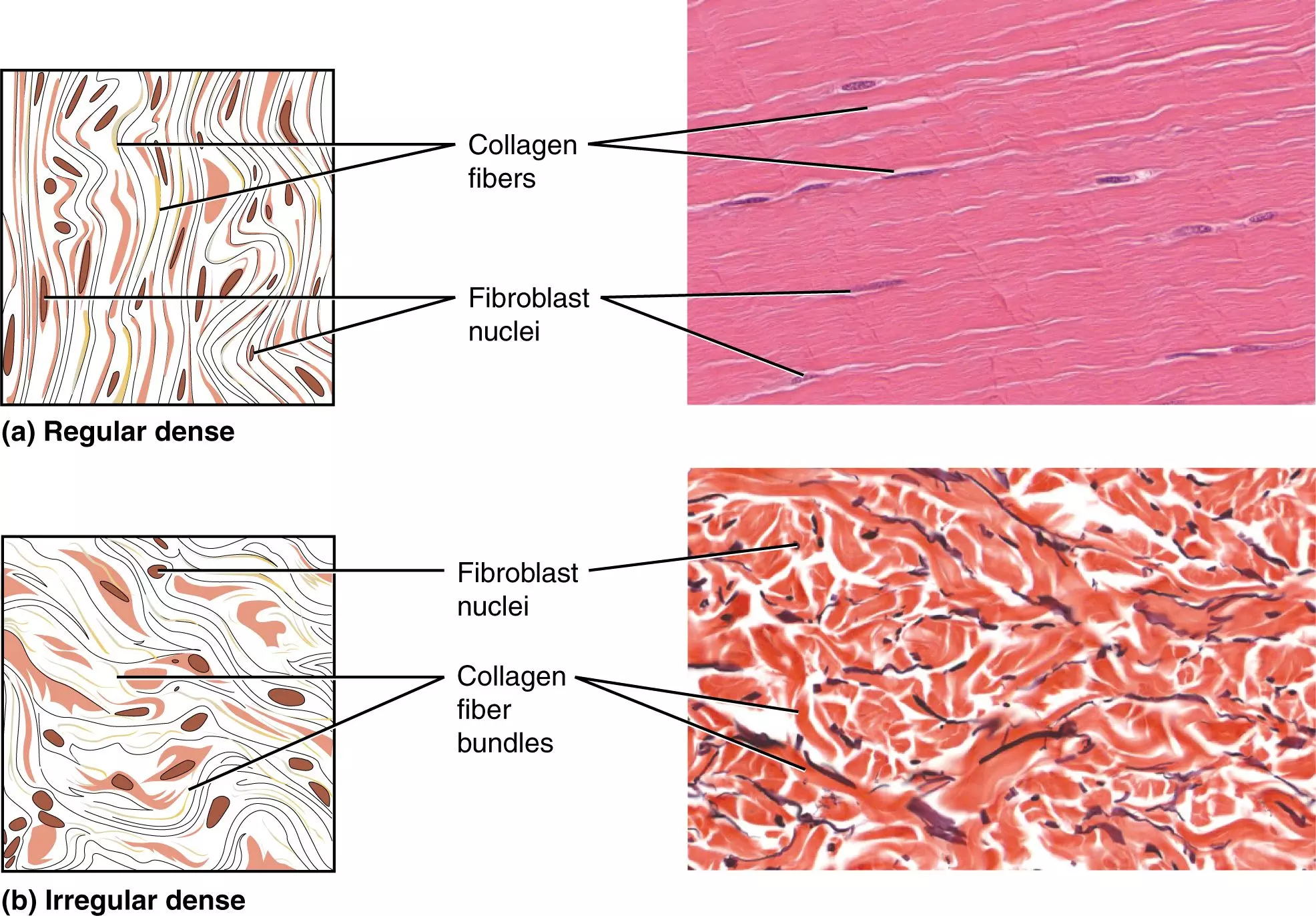
Image: The difference between regular and irregular dense connective tissue. Notice the parallel bundles of regular dense vs the seemingly random arrangement of irregular dense.
Creative Commons Image Source OpenStax College [CC BY 3.0 (https://creativecommons.org/licenses/by/3.0)]
Examples of connective tissues within the body:
Tendons
In tendons (connective tissue that connects muscles to bones) the collagen bundles lie in a parallel, densely packed formation in line with the tensile force exerted by the muscle. Rows of elongated flattened fibroblasts lie between the collagen bundles. These allow muscles to exert their force onto the bone and cause movement.
Ligaments
Ligaments (connective tissue that connects bone to bone) have collagen bundles which are densely packed in a parallel arrangement, but undulate and are arranged in fascicles, separated by loose connective tissue.
Aponeuroses
An aponeurosis is a flat sheet of regular connective tissue with bundles of fibres in one layer often arranged at 90-degree angle to those in adjacent layers. They are commonly found covering large areas of the body and providing structural support to areas such as the abdomen and back.
Dermis
The dermis is a dense irregular connective tissue, underlying the epidermis of the skin. The bundles of collagen are densely packed but irregularly arranged, such that they are orientated in multiple directions. The skin can therefore resist forces in multiple directions to prevent tearing. The elastic fibres allow a degree of stretch and a restoration to the original shape after the skin is bent or folded.
- 16594

