By Dr. Ethan Kavanagh and Dr. Ben Appleby
Next Lesson - The Infection Model
Core
An infectious disease is thus a disease that is caused by such an infection. Anytime you see the term “agent”, it is just referring to a micro-organism (also known as a microbe) that causes an infection.
There are five generic stages for how a microorganism, (in our example a bacterium) could cause an infection within a human:
This is known as the transmission of the microorganism and it is split into two broad categories:
- Direct contact transmission occurs when there is physical contact between an infected person and a susceptible person. For example- Most sexually transmitted infections (STIs) are transmitted in this way.
- Indirect contact transmission occurs when there is no direct human-to-human contact, but the susceptible patient comes into contact with a contaminated surface or object (a fomite). Transmission can also occur via vectors, which are living organisms that carry and transmit infection, such as mosquitoes, flies, mites, fleas and ticks. In indirect contact transmission, the susceptible person comes into contact with a contaminated object (fomite), such as a door handle that has been sneezed on, or with a vector, such as an Anopheles mosquito that has fed on an infected human.
2. Inhalation - involves the entry of infective microorganisms through the respiratory tract. This can be broadly split into airborne and droplet transmission. In airborne transmission, very small particles generated by coughing, sneezing or breathing can remain suspended in the air for prolonged periods. Droplet spread however has a much larger particle which when coughed or sneezed out will fly for a short distance before dropping to the floor or a surface which it may then contaminate.
3. Ingestion - involves the entry of infective organisms through the gastrointestinal system. It mainly consists of faeco-oral transmission which is usually when food or water contaminated with faeces is ingested. Although it is rare for individuals to knowingly directly ingest faeces, this may happen with microscopic amounts of faeces in cases of poor hand hygiene. A few examples of how this happens would be: drinking water contaminated with sewage, eating shellfish/raw fruit and vegetables that have been harvested or washed in contaminated water, sexual activity, or poorly managed/chlorinated swimming pools.

Image: High quality swimming pool management - anyone for a swim?
2. Adherence
Simply put adherence is the binding of a pathogen to a host cell. This is done using an adhesion protein, or ligand, on the bacterial cell wall or viral capsule surface, which then binds to a receptor (a carbohydrate structure bound to the lipid membrane) on a host cell.
Fimbriae are also believed to be involved in attaching some bacteria to a solid surface or another cell (there is a structural difference between pili and fimbriae but the terms are mostly used interchangeably) - this is one example of a virulence factor, a specific adaptation of a pathogen (organism capable of infection) that allows it to better infect cells, replicate and survive.
3. Invasion
Image: Mycobacterium tuberculosis is a pathogenic mycobacterium and is the causative agent of Tuberculosis.
Non-Phagocytic cell invasion
Bacteria that invade non-phagocytic cells work slightly differently by something called the zipper method. Using Yersinia pseudotuberculosis as an example, the bacterium will bind to a receptor that is involved in binding to other cells, which tricks the cell into forming a cell junction with it. The bacterium is relatively small compared to the host cell so the host cell tries to spread over the adhesive surface of the bacterium, endocytosing it (receptor-mediated endocytosis).
The other way bacteria infect nonphagocytic cells is by the trigger method. In short the bacterium injects molecules into the host cell which activates the Rho family of GTPases, that changes the shape of the actin cytoskeleton so it can fold over the bacterium and invaginate it.
4. Multiplication
Multiplication of bacteria is via the mechanism of binary fission. The process starts with replication of the main strand of circular DNA of the bacteria into two copies. The next step is the replication of any plasmids; small circular strands of DNA which contain any ‘luxury genes’ ie those not crucial in the basic functioning of the bacteria. Multiple copies of these plasmids may be made. The final step is when the main strand copies move to opposite poles of the cell, the bacteria pinches in the middle and finally divides into two.
In viruses, the host cell's multiplication machinery is taken over and used as a "factory" for further viruses to be produced based on the RNA/DNA of the initial virus which infected the cell. The copies are then released from the cell to infect further cells.
5. Dissemination
Dissemination involves the spreading of the bacteria/ viral load from one part of the body to another. For example, infection with TB, this is from the lungs to a secondary site (normally another organ) through the blood and lymphatics. Viruses released from body cells will circulate around the body looking for cell-surface receptors that they can bind to, in order to enter the target cell and begin multiplication again.
Commensal bacteria are part of the normal flora of the body and are generally harmless, however commensals can lead to pathology either by overgrowth, invasion or being destroyed.
Virulence is the ability of a micro-organism to infect a host (at all steps of the process), and virulence factors are what help the micro-organism do just that. General examples of these include toxins, haemolysins (proteins and lipids that cause lysis of erythrocytes (blood cells) by destroying their cell membrane) and proteases - but toxins are the easiest to understand.
As with any condition it is crucial that a history is taken. If an infective cause is suspected it is important to focus on some of these specific questions including
- Potential exposures a patient may have had which includes: travel history for the last 6-12 months, the calendar time (eg Norovirus as the winter vomiting bug), contact with any animals
- Relative time from exposure to presentation to indicate incubation time of the infection
- Vaccination history (don’t forget some people opt not to have their children vaccinated so it is important not to make assumptions)
- Symptoms of the presenting complaint (severity, duration, rash, radiation, muscular problems, numbness, vomiting, appetite etc)
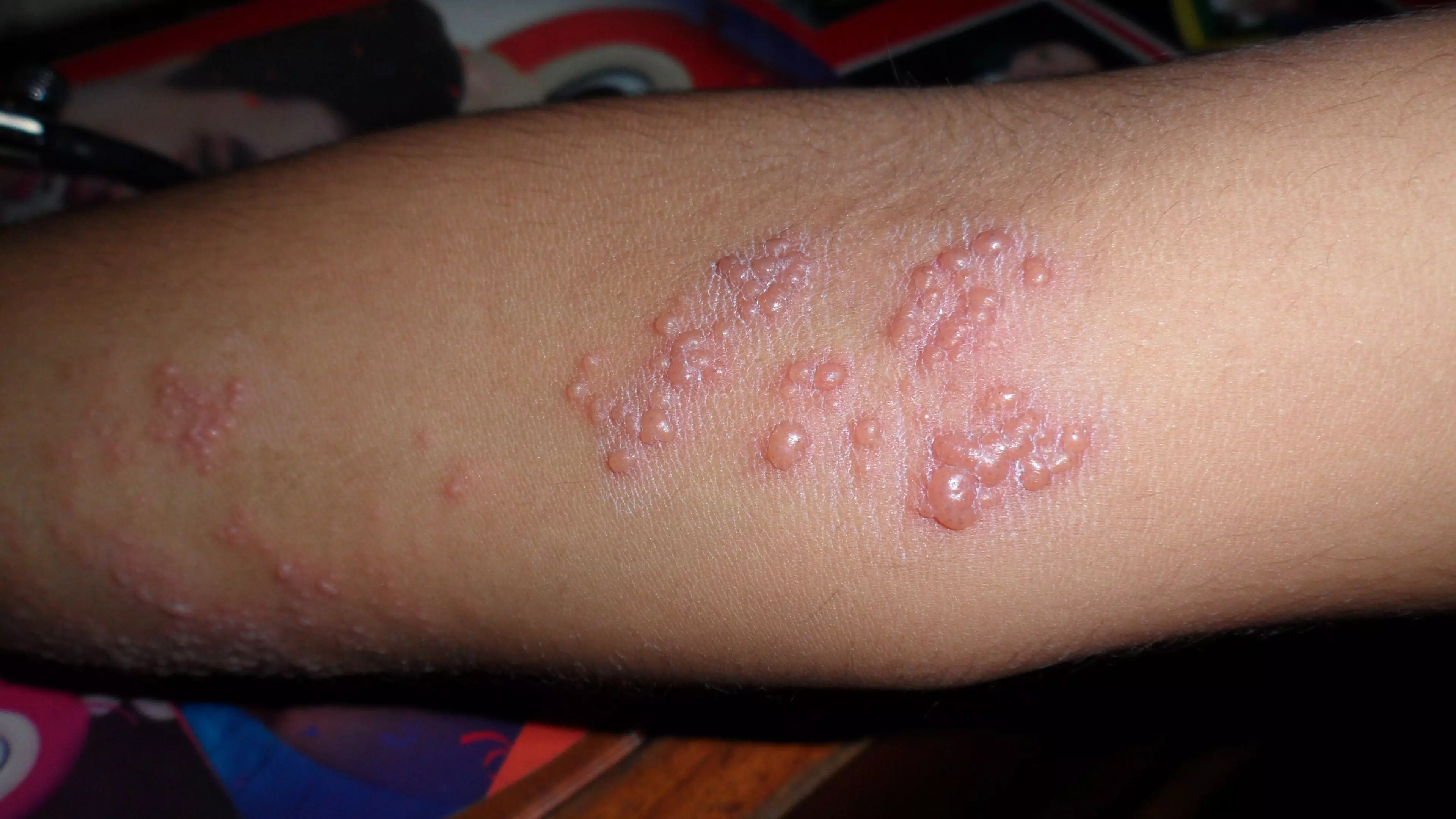
Image: Picture of Herpes zoster affecting the C7 dermatomal region of a patient’s elbow.
Meanwhile the rash associated with Neisseria Meningitidis is a non blanching (does not disappear when a tumbler/clear glass is rolled over it) petechial rash. Small differences in examination findings can lead to large changes in diagnosis.
Investigations
There are a variety of investigations that may be carried out to help determine the cause of an infection. Some of them are listed below:
- Full blood count - covered in Haematology
- C-reactive protein (a sign of systemic inflammation, produced by the liver)
- LFTs (liver function tests - sign of liver damage)
- U's and E's (urea and electrolytes - a sign of multiple issues, including kidney damage/failure)
- Imaging (X-ray, ultrasound, MRI)
- Blood cultures (to grow bacteria if it is present and potentially test it for antibiotic susceptibility)
- Antigen detection (of the micro-organism)
- Antibody detection (understand the patient’s response - particularly relevant in Hepatitis B)
- Nucleic acid and viral nucleic acid amplification testing (used to detect specific viruses or bacteria)
Edited by: Dr. Marcus Judgeand Dr. Ben Appleby
- 12531

