All done here! Check out our other subjects!
Abstract
- Checkpoints in the cell cycle exist to prevent genetically unstable cells from undergoing mitosis.
- There are two mechanisms by which a double-strand break can be repaired: Non-homologous end joining, and homology directed repair.
- Cancer cells exhibit faulty DNA repair mechanisms.
- New chemotherapy approaches aim at inhibiting the only DNA repair mechanisms which are active in cancer cells, which still leave healthy cells with some active DNA repair mechanisms.
Core
Central Factors of DNA Damage Response
DNA damage response is a hugely complex area of genetics. Thankfully, there isn’t too much detail that is required for medical training.
In general, replication stress (where the replication fork slips, stalls or breaks) and mutagens cause DNA damage. This activates a signalling cascade which either results in the cell undergoing senescence/apoptosis or DNA being repaired at the next cell cycle checkpoint.
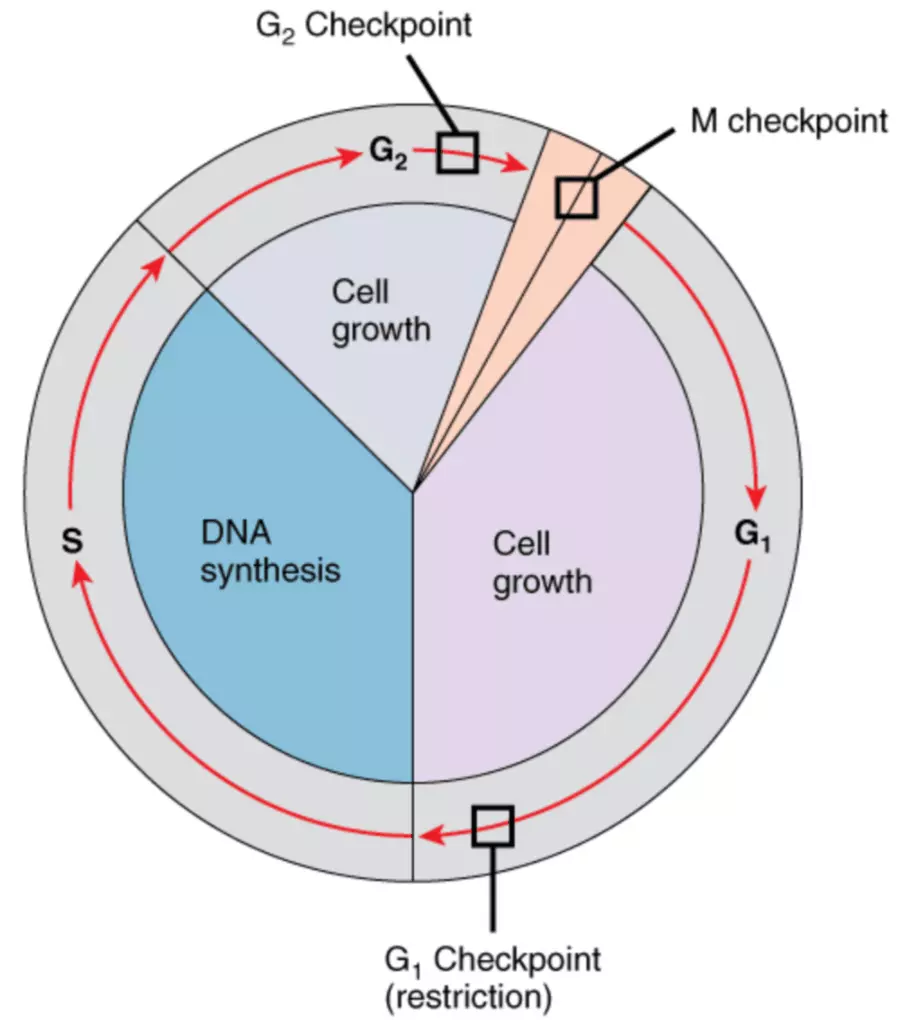
Diagram: The stages and checkpoints of the Cell Cycle
Creative commons source by OpenStax, edited by Dr. Joshua Sturgeon [CC BY 4.0 (https://creativecommons.org/licenses/by/4.0)]
The above image shows the cell cycle with each stage of interphase marked along with mitosis (in pink). This image also highlights where certain cell cycle checkpoints are located. Checkpoints are periods of temporary cell cycle arrest which provide time for DNA damage to be repaired.
The mitosis (M) checkpoint checks to make sure that all chromosomes are properly attached to the mitotic spindle. If this happens correctly, then duplicated chromosomes can then be pulled apart.
The G1 checkpoint checks to make sure the intracellular environment is favourable for DNA synthesis. If the environment is favourable, then DNA synthesis can begin.
The G2 checkpoint checks to make sure that all DNA is replicated and checks to see if all DNA damage has been repaired. If this is true, the cell can then undergo mitosis.
In healthy cells, these checkpoints work to ensure the cell remains healthy and can go through mitosis.
If DNA damage levels are too high and cannot be adequately repaired, p53-mediated signalling can cause the cell to arrest the cell cycle, allowing time for repair, or trigger apoptosis or senescence. Loss of p53 function allows damaged cells to progress through checkpoints inappropriately.
Ideally, all DNA damage will be repaired, and cell function will be maintained. However, this is not always possible.
There are multiple DNA repair pathways, the type of pathway used depends on the type of DNA damage and the cell cycle phase.
One way in which DNA can be damaged is through a double-strand break. As the name suggests, both strands of DNA have broken, making this the most genotoxic DNA lesion. Although the fine details of repair pathways do not need to be memorised and only a general understanding is required, we have included this information for reference.
There are two ways in which a double-strand break can be repaired:
Non-Homologous End Joining (NHEJ):
- DNA has a double-strand break.
- Proteins called KU70/80 move to the exposed ends of DNA and act as caps to protect them.
- DNA protein kinases (DNA-PKs) move to the ends of DNA and form a DNA-PK complex. These process the ends of the DNA strands and remove damaged DNA if required.
- Other proteins e.g. DNA Ligase IV are recruited to ligate the two ends of DNA back together.
- This is a more complicated repair mechanism and has multiple sub-pathways.
- Firstly, the exposed ends of DNA are resected.
- This mechanism utilises a homologous template - which essentially means an undamaged copy of the DNA involved in the double-strand break - e.g. a sister chromatid.
- In many models, strand invasion occurs between the broken DNA and the homologous template, which may involve formation of a Holliday junction.
- The Holliday Junction is then nicked complete the repair.
The image below shows both mechanisms in detail much greater than what is needed for pre-clinical exams but are good to help you visualise the repair mechanisms.

Diagram: NHEJ and Homology-directed repair in detail
Creative commons source by Hannes Lans, Jurgen A Marteijn and Wim Vermeulen [CC BY 2.0 (https://creativecommons.org/licenses/by/2.0)]
DNA Repair: Relevance to Cancer
The two hit hypothesis explains how cells accumulate mutations over time. If a mutation damages a tumour suppressor gene such as p53 the cell should be fine as the second copy of the gene will be unaffected. However, if a second ‘hit’ is given and there is no tumour suppression, the cell can go from being healthy to pre-malignant and then finally malignant. This process is called carcinogenesis.
Abnormal DNA damage responses can be inherited, which will predispose an individual to cancer in later life e.g. Hereditary Nonpolyposis Colorectal Cancer, also known as Lynch syndrome. Lynch syndrome is caused by a defect in DNA mismatch repair and as a result leads to a higher likelihood of cancer.
Once a cancer develops, cells can continue to mutate. This leads to intra-tumour heterogeneity which makes tumours harder to treat as it can lead to therapy resistance or metastasis.
Take for example, a highly heterogeneous tumour. Some cells in this tumour are highly sensitive to one form of chemotherapy, whereas other cells are resistant to it. After chemotherapy, the cells which were sensitive will have died, but this leaves space for the resistant cells to grow. This means the chemotherapy is less effective overall as only the resistant cells are left in the tumour. This is called clonal expansion.
An alternative result to clonal expansion is chemotherapy-induced mutagenesis. This occurs when cells are not killed outright by the chemotherapy, but their DNA is damaged just enough to mutate. This is a problem as it further increases the heterogeneity of the tumour.
At the moment, the most well-established approach to treating cancer is to cause more DNA damage, as the cancer cells already have defects in their DNA repair mechanisms so will be pushed into apoptosis with extreme damage. However, normal physiologically rapidly dividing cells are also often affected, which cause various side effects:
- Radiation:
- Skin problems
- Fatigue
- Heart problems
- Chemotherapy:
- Hair Loss
- Fertility Problems
- Nausea
Cancer treatment can also promote tumour evolution and secondary cancers.
At the moment, targeted chemotherapy options are being explored, which seek to inhibit only a few repair pathways which are active in tumour cells. As normal cells have all DNA repair pathways functioning, these cells will survive. However, this approach is often limited to a specific context or cancer type. This technique of only targeting tumour cell pathways is known as synthetic lethality.
For more information about cancers, head to the Neoplasia articles in our Pathology series.
Edited by: Dr. Ben Appleby and Dr. Maddie Swannack
Reviewed by: Dr. Marcus Judge
- 8677

