Next Lesson - Conditions of the Thigh
Abstract
The conditions of the knee included in this article are:
- Infra-patellar bursitis - Clergyman’s knee
- Pre-patellar bursitis - Housemaid’s knee
- Supra-patellar bursitis - Knee effusion
- Osgood-Schlatter’s disease
- Patella fracture
- Patella dislocation
- Septic arthritis of the knee
- Cruciate ligament tears
- Collateral ligament tears
- Menisci tears
- Unhappy triad
Core
Want more information on anatomy before you begin looking at conditions? Head to our articles on Bones of the Lower Limb, Muscles of the Thigh and Muscles of the Lower Leg for more information!
Infra-patellar bursitis is also known as ‘Clergyman’s knee’. This is inflammation of the infra-patellar bursa (a fluid-filled sac that counters friction at a joint and sits just below the patella) due to repeated micro trauma often caused by upright kneeling (classically in the clergy). Infra-patellar bursitis presents as a painful, erythematous swelling below the knee joint.
Infra-patellar bursitis is usually treated with rest, ice, elevation and over the counter painkillers. However, if this is unsuccessful and infection is suspected, aspiration may be taken from the bursa and tested for infection. If there is an infection present, antibiotics will be prescribed and if not, a steroid injection may be given to reduce the swelling at the affected joint. If the bursitis is severe or keeps returning, the bursa may need to be surgically drained/removed but this is very rare.
Pre-patellar bursitis is also known as ‘Housemaid’s knee’. This is inflammation of the pre-patellar bursa (a fluid-filled sac that counters friction at a joint and sits in front of the patella) due to repeated micro trauma or a fall. This condition presents as a painful, erythematous swelling directly over the knee joint. It is called ‘Housemaid’s knee’ because it can occur with repeated kneeling forwards e.g. to scrub a floor by hand.
Pre-patellar bursitis is usually treated with rest, ice, elevation and over the counter painkillers. However, if this is unsuccessful, the bursa may be aspirated and tested for infection. If there is an infection present, antibiotics will be prescribed and if not, a steroid injection may be given to reduce the swelling at the affected joint. If the bursitis is severe or keeps returning, the bursa may need to be surgically drained/removed but this is very rare.
Supra-patellar bursitis is inflammation of the suprapatellar bursa, which communicates with the synovial cavity of the knee joint. This can be caused by: osteoarthritis, rheumatoid arthritis, infection, gout or injury to the ligaments or menisci of the knee. This condition presents with a painful, erythematous swelling above the patella and below the quadriceps muscle.
Treatment of supra-patellar bursitis is dependent on the cause, but rest, ice, elevation and over the counter painkillers are often recommended.
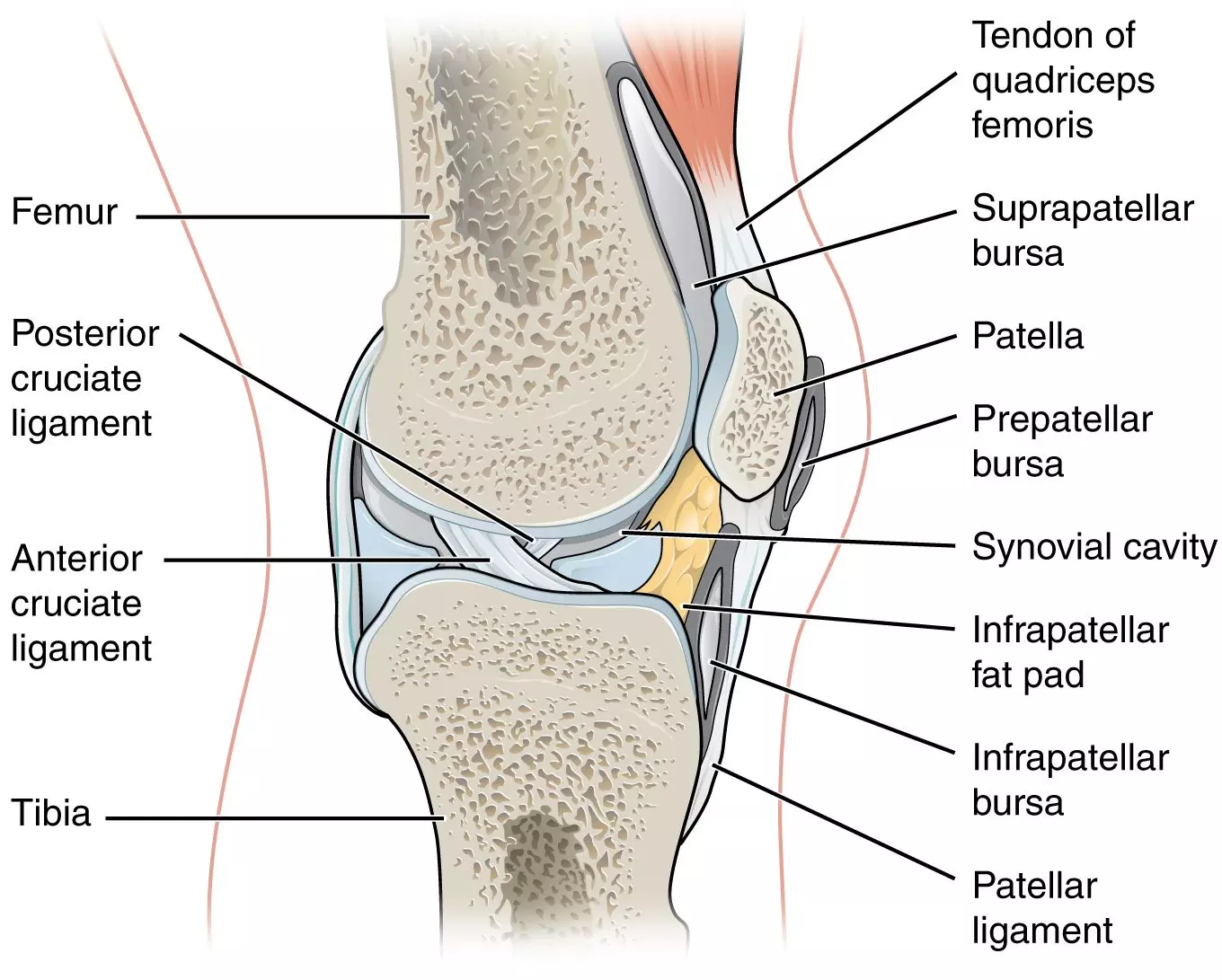
Diagram - The bursa surrounding the knee joint
Creative commons source by OpenStax College [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)]
Osgood-Schlatter’s disease is inflammation of the patellar ligament, often referred to clinically as the patellar tendon, at its insertion into the tibial tuberosity. This condition is common in teenage athletes. It presents with localised pain and swelling and in 20-30% of cases, symptoms are bilateral.
Treatment is generally rest, ice, elevation and over the counter painkillers, plus exercises to stretch and strengthen the tendon. Typically, symptoms completely resolve with age as the growth plate closes, but it can be difficult to enforce rest in the typical patient, reducing effective healing.
Fractures of the patella are often caused by direct impact or indirect eccentric (not central) contraction of the quadriceps (contraction to straighten the leg when the knee is not straight below the hip but deviated to the side). They are most commonly seen in 20-50 year olds and usually present with: swelling (due to bleeding at the site of fracture), a palpable defect and an inability to perform a straight leg raise (if patella fracture is displaced).
Treatment of a non-displaced patella fracture is to use a long leg cast or knee immobiliser to allow the patella to remain in the correct position while it heals. If the patella fracture is displaced, surgery is the most likely option for treatment. In both cases physiotherapy may be required to return the leg to full function, once it can bear weight again.
It is important to bear in mind that a bipartite patella can be a normal finding, particularly in adolescents. In a young person presenting with a patella in two parts on imaging, this does not always represent an acute fracture, and management should be guided by the clinical history and examination.
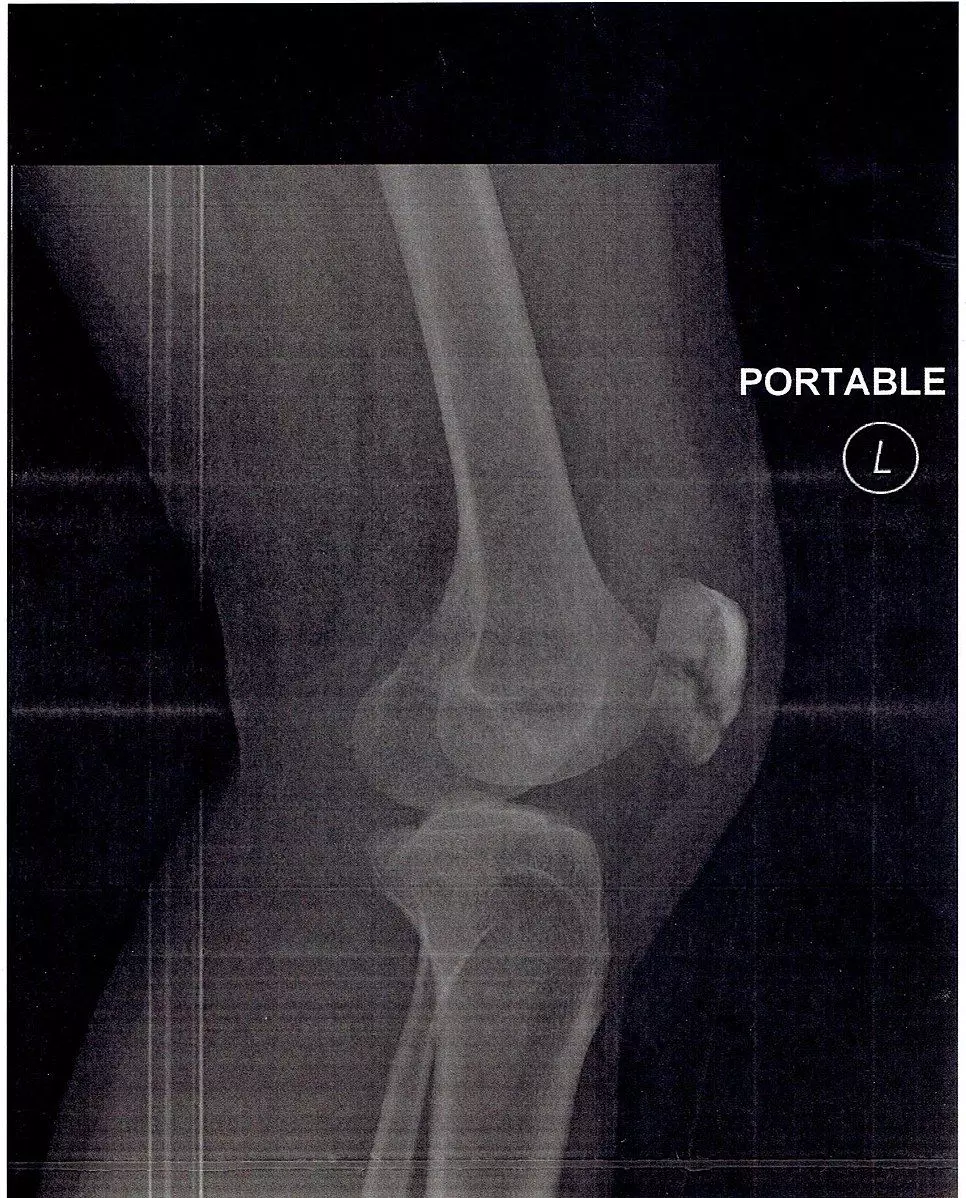
Image - An X-ray of a patella fracture
Creative commons source by Carlo Joseph Moskito [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)]
Dislocation of the patella most commonly occurs laterally due to internal rotation of the femur on a flexed knee. It most often occurs in athletic teenagers who try to change direction when running on a flexed knee. It usually presents with: severe knee pain, swelling, an inability to straighten the knee and sometimes a ‘popping’ sensation is experienced.
Treatment is reduction of the kneecap. During reduction pain relief is given. After reduction an X-ray may be done to check the patella is in the correct place and that there is no other damage. The leg will usually be immobilised with a splint initially and physiotherapy may be recommended to aid recovery.
A knee effusion occurs when excess fluid collects around the knee joint. It occurs commonly following an injury to the knee, when the joint produces excess fluid to protect the knee from further injury but can also be caused by osteoarthritis or infection.
Diagnostic tests include aspiration of the knee joint to help determine the cause of the swelling, and imaging to help rule out bony or ligamentous injury. The treatment of a knee effusion depends on the cause, for example giving antibiotics if an infection is present. However, management depends on the cause. Rest and simple analgesia may be appropriate in some cases, but suspected infection requires urgent assessment and treatment.
Septic arthritis is the invasion of joint space by microbes. It can occur elsewhere in the body but is most commonly seen in the knee joint and can present like a knee effusion. Risk factors include: increasing age, rheumatoid arthritis, diabetes, immunosuppression, IV drug use and prosthetics in the knee (from a joint replacement). This condition presents with a fever; pain, swelling and erythema around the knee; and a decreased range of motion.
A joint aspirate is taken and cultured to determine the bacterial cause of the infection (usually Staphylococcal or Streptococcal bacteria) and then antibiotics are used to treat the infection. If particularly severe, the fluid in the joint may also need to be drained.
Anterior cruciate ligament (ACL) tears usually occur due to quick deceleration, hyperextension or rotation (e.g. with a sudden change of direction), or due to a blow to the back of a flexed knee. In an ACL injury, the tibia slides anteriorly under the femur.
Posterior cruciate ligament (PCL) tears usually occur due to an external force on a flexed knee (a ‘dashboard injury’) or due a fall onto a flexed knee with a plantar-flexed ankle. In a PCL injury, the tibia slides posteriorly under the femur.
Cruciate ligament tears normally present with: a ‘popping’ sensation, severe pain, rapid swelling, reduced range of motion and a feeling of instability when weight bearing. They can be tested by the drawer test (for both ACL and PCL tears) and Lachman’s test (ACL only).
Treatment can range from RICE (rest, ice, compression and elevation) to surgery to reconstruct the ligament with a section of tendon from elsewhere if needed.
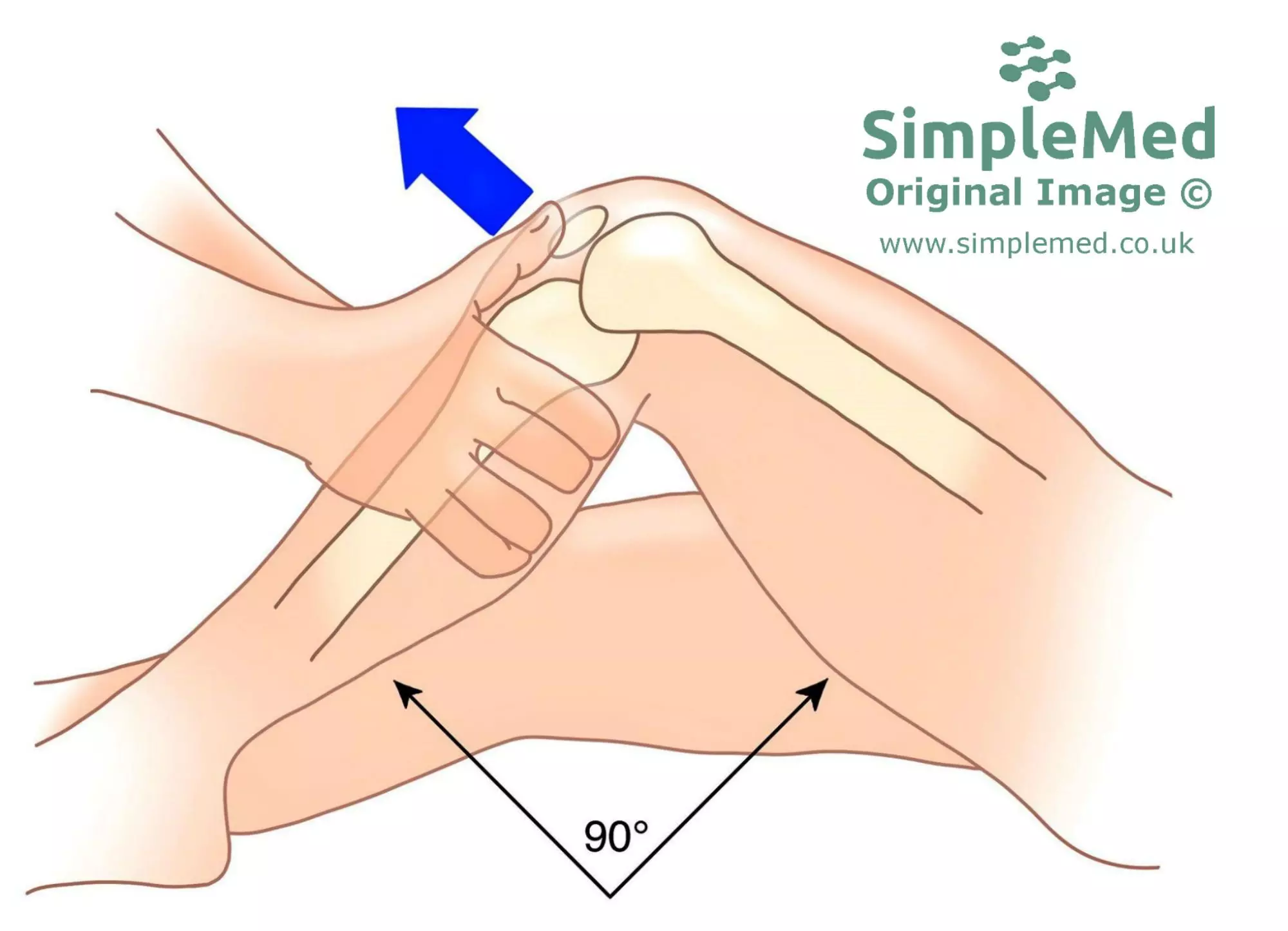
Diagram - The anterior drawer test
SimpleMed original by Dr. Bethany Turner
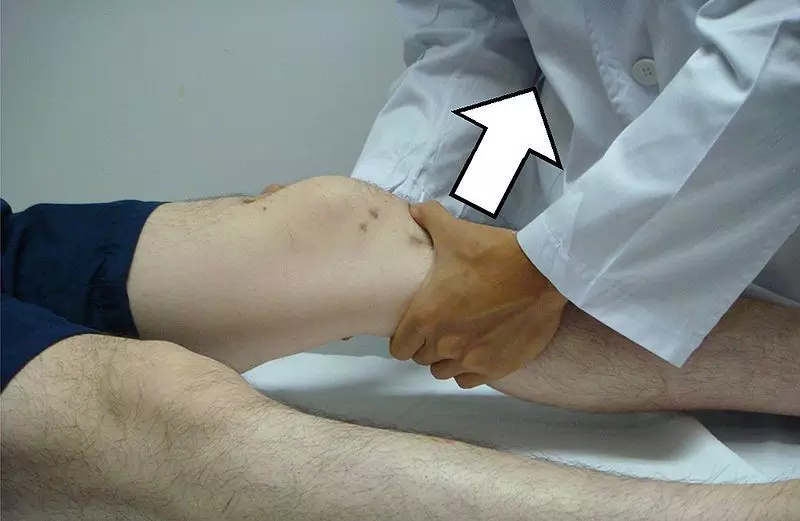
Image - A demonstration of Lachman's test
Creative commons source by Lam et al. Sports Medicine, Arthroscopy, Rehabilitation, Therapy & Technology 2009 [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)]
Collateral ligament tears are a common sporting injury that occur due to a direct blow to the side of the knee. A varus deformity occurs when the knee is forced outward due to a medial blow, resulting in lateral collateral ligament damage. A valgus deformity occurs when the knee is forced inward due to a lateral blow, resulting in medial collateral ligament injury.
Medial collateral ligament tears are more common because a blow to the lateral side of the knee is easier to obtain than a blow to the medial knee. This condition presents with pain, stiffness and instability and pain is increased when either a varus or valgus stress test is performed. The majority of collateral ligament tears can be treated with ice, painkillers, bracing and strengthening exercises but occasionally surgery may be required.
A torn meniscus is one of the most common knee injuries and is often caused by forceful rotation of the knee. It often occurs in young athletes but can occur in the elderly with little or no trauma because of degenerative changes to the knee. This condition usually presents with: intermittent pain at the joint line, a clicking, catching or locking sensation and reduced movement causing instability.
Treatment can range from RICE (rest, ice, compression and elevation) and strengthening exercises to surgery (either for repair or to trim meniscus to reduce symptoms).
The unhappy triad is also known as a ‘blown knee’. It describes a combined injury to the ACL, medial collateral ligament and medial meniscus due to a blow to the lateral knee. It is a very severe injury and can permanently reduce the function of the knee.
If mild, RICE and strengthening exercises may be sufficient to treat this condition but often arthroscopic surgery may be required to repair the torn structures (ACL and medial meniscus as MCL usually heals on its own). Physical therapy is an important part of recovery whether surgery is required or not.
Reviewed by: Dr. Thomas Burnell
Edited by: Dr. Maddie Swannack
- 8306

