All done here! Check out our other subjects!
Abstract
- Routes for metastasis of malignant tumours include via blood, lymphatics and body cavities (e.g. peritoneum and pleura).
- Local effects of tumours include compression and obstruction of surrounding structures.
- Systemic effects of tumours include paraneoplastic syndromes, such as ectopic hormone secretion, as well as effects related to increasing tumour burden.
Core
Invasion is when a tumour grows from its primary site into surrounding structures.
Epithelial to mesenchymal transition (EMT) is a process by which epithelial cells undergo multiple changes until they more closely resemble a mesenchymal cell. These changes reduce cell adhesion and increase motility which facilitates invasion.
For malignant cells to invade into surrounding tissues they require:
- Altered cellular adhesion
- Decreased expression of E-cadherin reduces the cell-cell adhesion.
- Changes to expression of integrin receptors alters the adhesion between cells and extracellular matrix.
- Increased secretion of proteolytic enzymes
- Matrix metalloproteinases (MMPs) are enzymes secreted by malignant cells to enable them to breakdown surrounding connective tissue.
- Increased cellular motility
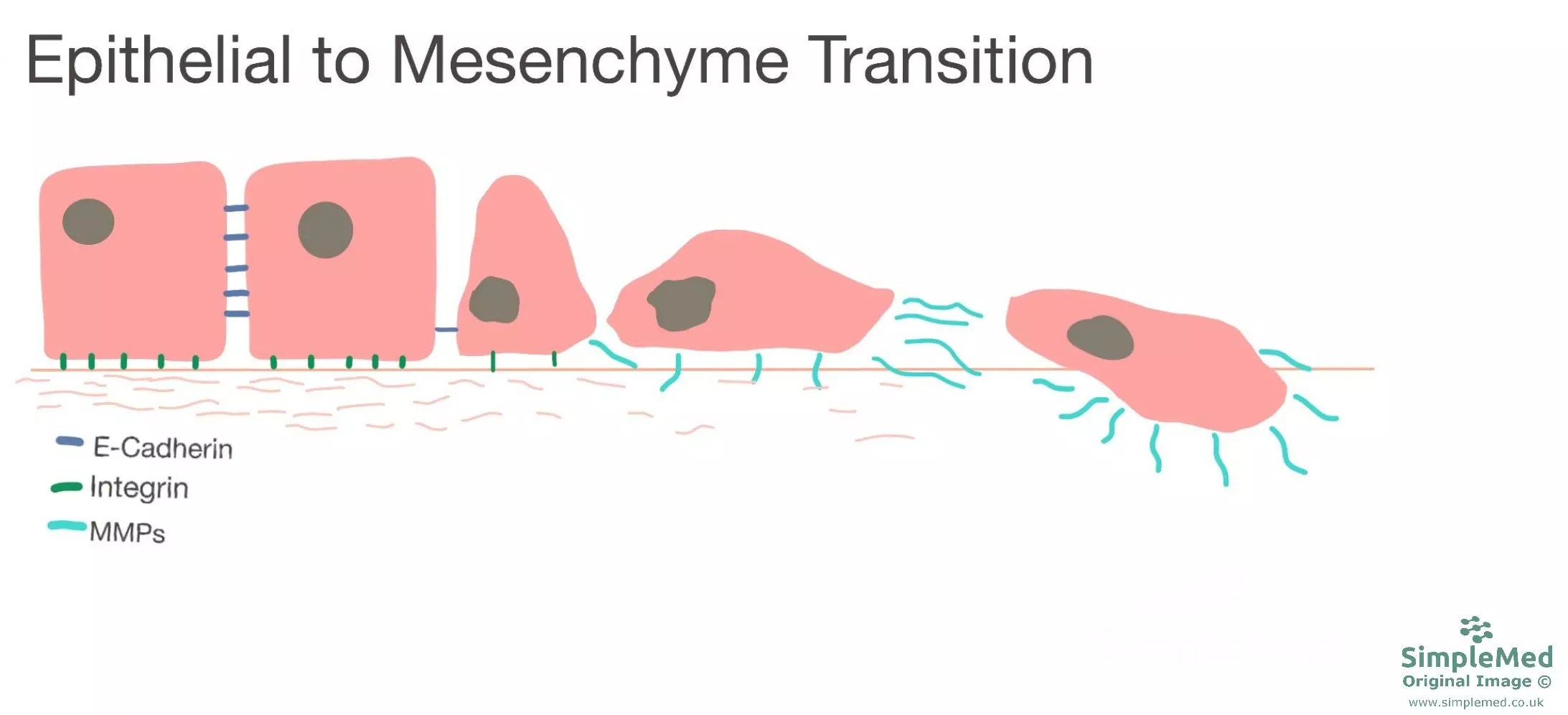
Diagram - The progression of epithelial to mesenchymal transition which eventually allows epithelial cells to cross the basement membrane and invade surrounding structures. (MMPs - matrix metalloproteinases)
SimpleMed original by Dr. Emily Smith
Metastasis is the process in which malignant cells migrate from the primary site of the tumour to a distant secondary site to form another tumour. It is a consequence of growth and invasion at the primary site. In order to metastasise, malignant cells need to:
- Invade through the basement membrane of blood or lymphatic vessels - intravasation.
- Avoid host immune defences.
- Attach to endothelium at a distant location.
- Leave the blood or lymphatic vessel to enter surrounding tissue - extravasation.
There are several different routes of metastasis; bloodstream, lymphatics and transcoelomic spread (across a body cavity such as through the peritoneal, pleural or pericardial cavities). Carcinomas typically spread to the draining lymph nodes first, and then spread via the blood stream. Sarcomas tend to spread by the blood stream first.
Many malignant cells can reach a secondary site but might not grow for a number of reasons, including being caught by the immune system, or not being able to invade through local cells. This spread of cancer cells leads to micro-metastases - clinically undetectable groups of malignant cells. These micro-metastases can start to regrow after a period of time, which is what causes an apparently cured patient to relapse. This is also the reason why patients with cancer cannot donate their organs.
Blood Stream Metastasis
Secondary tumours form in organs which are perfused by blood that has drained from the site of the tumour. For example, GI malignancies often spread to the liver due to drainage by the portal vein which takes blood to the liver.
Metastases through the blood often form masses at the liver, lungs, bone and brain due to blood flow patterns.
Bone is commonly favoured by carcinomas originating from lung, breast, thyroid, kidney and prostate. Metastases from the former four organs cause lytic lesions which means they decrease bone mass, whereas metastases from the prostate causes sclerotic lesions - increase bone mass. These changes can be visible on x-rays.
Lymphatic Metastasis
Malignant cells enter lymph nodes through the afferent lymph vessels and settle at the periphery of the node. They grow inwards and the node is gradually replaced by cancer cells and connective tissue. This can result in lymphadenopathy and blockage of lymph flow leading to lymphoedema in the region drained by the blocked lymph vessels.
Transcoelomic Spread
This type of metastasis occurs within pleural, pericardial and peritoneal cavities. This results in formation of a protein rich effusion (exudate) within the cavity. This fluid also contains malignant cells causing the exudate, so the fluid can therefore be aspirated and used for diagnosis.
Peritoneal effusions (ascites) are commonly caused by ovarian tumours, although can also be caused by any abdominal tumour. Pleural and pericardial effusions are often caused by breast and lung cancers.
Growth of benign and malignant tumours can lead to compression and obstruction of adjacent structures. For example, growth of a pituitary adenoma can cause compression of the optic chiasm, resulting in a bitemporal hemianopia - loss of peripheral vision. Colorectal carcinoma can cause constipation due to obstruction of the lumen of the bowel.
There are some local effects which are more specific to malignant neoplasms. Malignant neoplasms on mucosal surfaces often ulcerate and bleed, therefore GI malignancy is an important differential in older people presenting with anaemia. The bleeding could be occult (not visible to the naked eye) so patients may not realise.
A key feature of malignant neoplasms is their ability to invade into surrounding tissues. For example, at late stages cervical cancer can invade into the bladder and rectum, leading to fistula formation and incontinence as urine or faeces leak out of the vagina.
A paraneoplastic syndrome is a clinically detectable systemic effect caused by a neoplasm but not related to metastasis. These signs and symptoms are typically caused by ectopic hormone secretion, immune cross-reactivity, or cytokine release rather than the direct effects of tumour growth.
An increase in tumour burden, and other factors such as release of cytokines, can lead to cachexia (weakness and wasting), malaise, immunosuppression and thrombosis.
Tumours that secrete hormones can cause a range of effects. For example, a benign tumour of an endocrine gland may secrete hormones at a higher level than is secreted by healthy tissue - a thyroid adenoma secreting high levels of thyroid hormone results in thyrotoxicosis (hyperthyroidism), and an adenoma of the adrenal cortex can result in Cushing’s syndrome due to excess cortisol secretion.
Some malignant tumours are also able to produce hormones. This is called ectopic hormone secretion as they are not normal sites for hormone production. Examples of this include:
- Bronchial small cell carcinoma (a type of lung cancer) producing ACTH resulting in Cushing’s syndrome.
- Bronchial small cell carcinoma producing ADH resulting in Syndrome of Inappropriate ADH (SIADH).
- Bronchial squamous cell carcinoma producing a PTH related peptide (PTHrP), resulting in hypercalcaemia.
Tumour markers are substances released into circulation by tumour cells. They can be measured in the blood or urine, and their levels can be measured to monitor tumour burden and response to treatment. They are not usually used for diagnosis, but for tracking the established cancer.
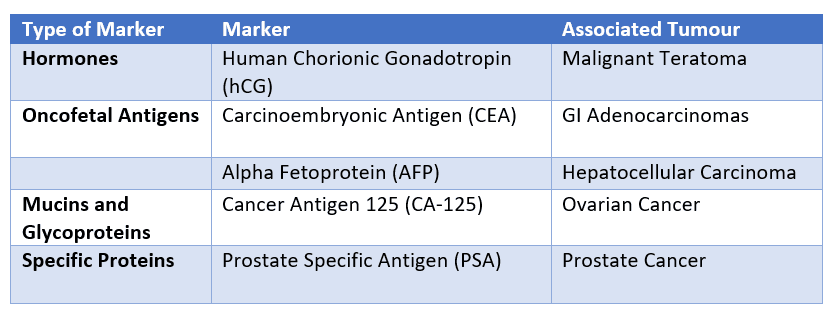
Table - Some tumour markers and their associated tumour
SimpleMed Original by Dr. Emily Smith
Edited by: Dr. Bethany Turner
Reviewed by: Dr. Maddie Swannack
- 9035

