All done here! Check out our other subjects!
Abstract
- The autonomic nervous system is responsible for the body’s involuntary functions.
- The autonomic nervous system has three major divisions: sympathetic, parasympathetic, and enteric.
- An autonomic neural pathway is a chain of two neurons: a pre-ganglionic and a post-ganglionic neurone.
- The sympathetic and parasympathetic nervous systems use different neurotransmitters, which act on their respective receptors.
- Actions of the sympathetic nervous system are associated with ‘fight or flight’.
- Actions of the parasympathetic nervous system are associated with ‘rest and digest’.
- We can use drugs which target the autonomic nervous system for therapeutic benefit.
- Overstimulation of the parasympathetic nervous system can lead to SLUDGE syndrome.
Core
What is the Autonomic Nervous System?
The autonomic nervous system (ANS) is the division of the body’s nervous system which controls all involuntary functions - e.g. heart rate, blood pressure, digestion, pupil diameter. It is separate from the somatic motor system, which deals with voluntary actions (i.e. skeletal muscle contraction).
The autonomic nervous system primarily controls involuntary motor output to organs, but it also includes visceral afferent fibres that carry sensory information from the periphery to the central nervous system. These inputs are integrated largely within the brainstem and hypothalamus.
The autonomic nervous system has two major divisions that are usually considered in this context:
- Sympathetic Nervous System (SNS) - Responsible for the ‘fight or flight’ response, triggered by stressful situations.
- Parasympathetic Nervous System (PNS) - Regulates basal activities, ‘rest and digest’.
Organisation of the Autonomic Nervous System
The division of the ANS into the sympathetic and parasympathetic systems is purely anatomical:
- SNS - Arises from the thoracic and lumbar divisions of the spinal cord (thoraco-lumbar outflow).
- PNS - Arises from the brainstem and sacral spinal cord (cranio-sacral outflow).
Remember the nervous system is bilaterally symmetrical, so when considering one side it is important to appreciate that the same is happening on the other side.
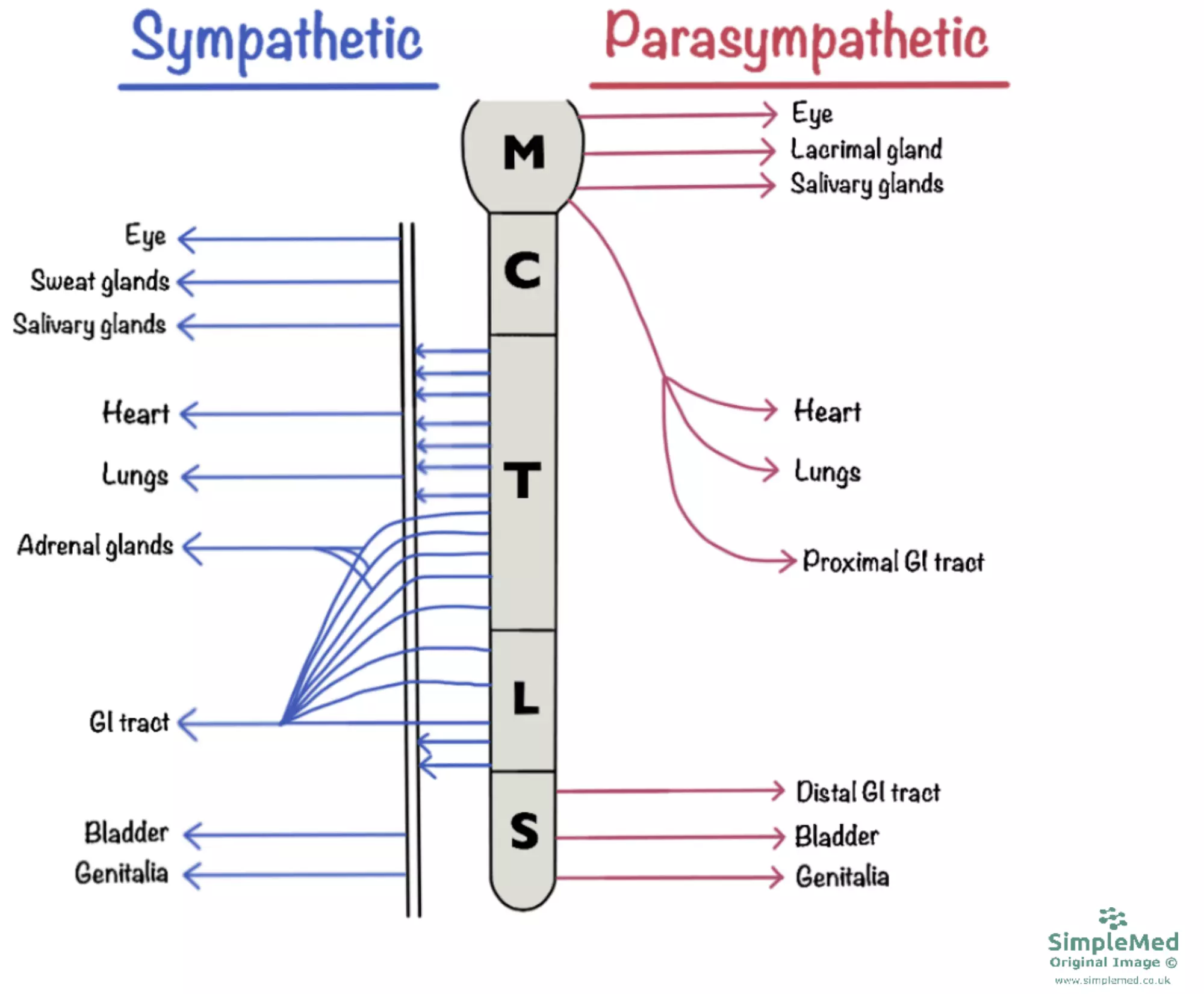
Diagram - The basic anatomy of the autonomic nervous system
SimpleMed original by Dr. Joshua Bray
Put simply, the autonomic nervous system is a chain of two neurones: a myelinated pre-ganglionic and an unmyelinated post-ganglionic neurone. A ganglion is a collection of neurone cell bodies and is where the pre-ganglionic neurone synapses onto the post-ganglionic neurone.
In the sympathetic nervous system:
- The pre-ganglionic neurone is relatively short and normally synapses within a specialised chain of sympathetic ganglia adjacent to the vertebral column - This is known as the sympathetic chain (or paravertebral chain).
- The post-ganglionic neurone is relatively long and exits the sympathetic chain to travel to the target tissue.
In the parasympathetic nervous system:
- The pre-ganglionic neurone is relatively long and travels along cranial nerves (e.g. vagus nerve), or as the pelvic splanchnic nerves if arising from the sacral cord - They synapse close to or even within the wall of the target tissue.
- The post-ganglionic neurone is consequently relatively short.
Actions of the Autonomic Nervous System
As covered in previous articles, neurones communicate with other cells at synapses, where they release a neurotransmitter which activates receptors on the post-synaptic membrane.
All pre-ganglionic neurones (both sympathetic and parasympathetic) use acetylcholine (ACh) as their neurotransmitter. The acetylcholine acts on nicotinic acetylcholine receptors on the membrane of the post-ganglionic neurone.
For post-ganglionic neurones, the use of neurotransmitter differs between sympathetic and parasympathetic divisions:
- Sympathetic post-ganglionics release noradrenaline, which acts on adrenoceptors on the membrane of the target cell.
- Parasympathetic post-ganglionics release ACh, which acts on muscarinic acetylcholine receptors on the membrane of the target cell.
Adrenoceptors and muscarinic receptors are examples of G-protein coupled receptors (GPCRs). For more information, check out our article on G-Protein Coupled Receptors.
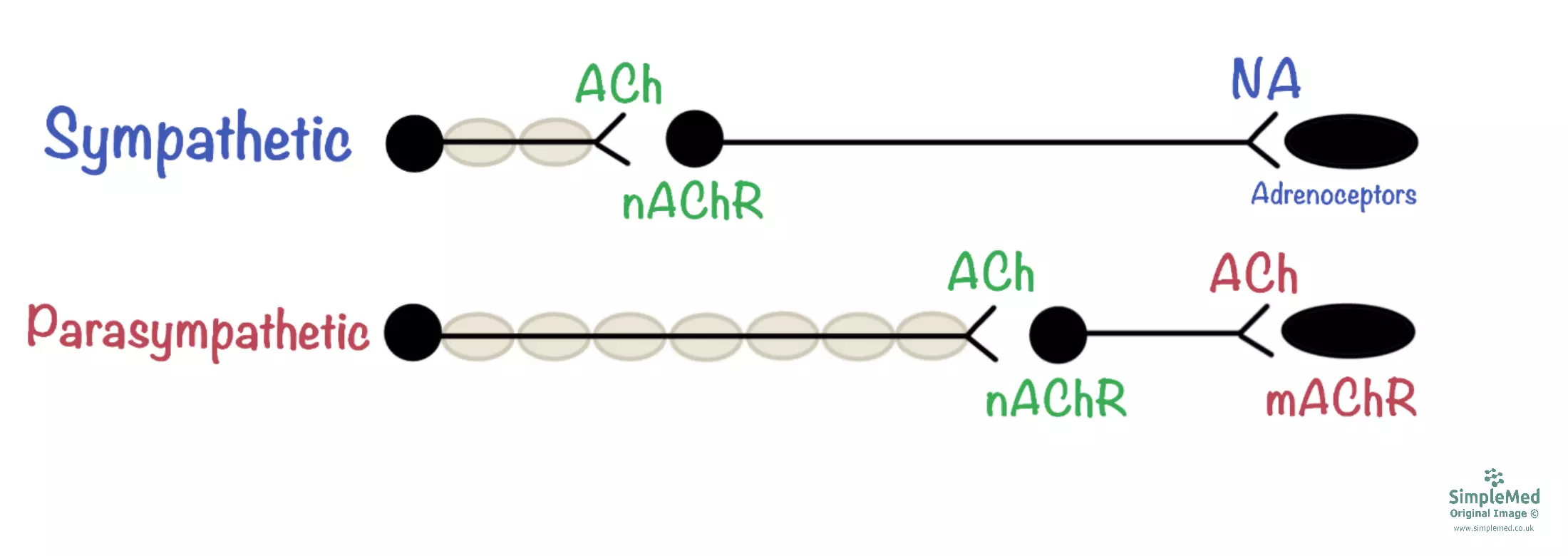
Diagram - The communication between pre- and post-ganglionic neurones of the autonomic nervous system
SimpleMed original by Dr. Joshua Bray
Stimulation of the sympathetic nervous system can result in:
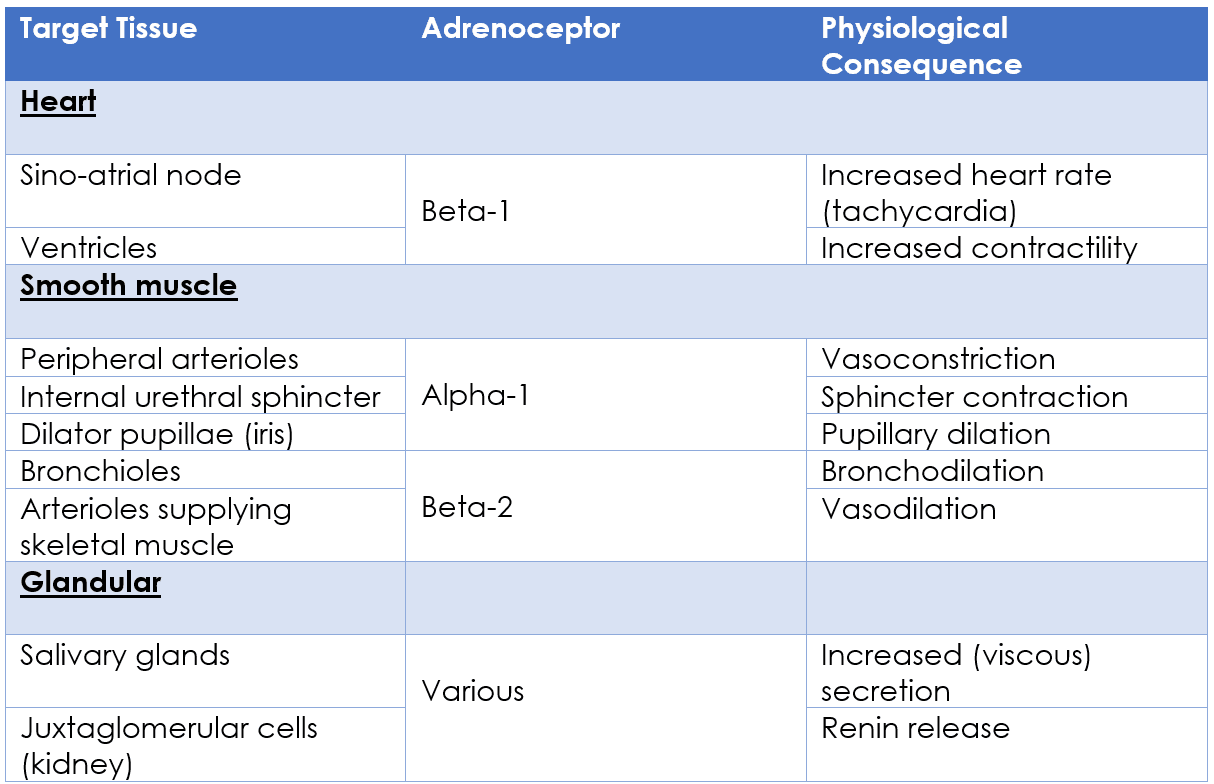
Table - The physiological actions of the sympathetic nervous system
SimpleMed original by Dr. Joshua Bray
Stimulation of the parasympathetic nervous system can result in:
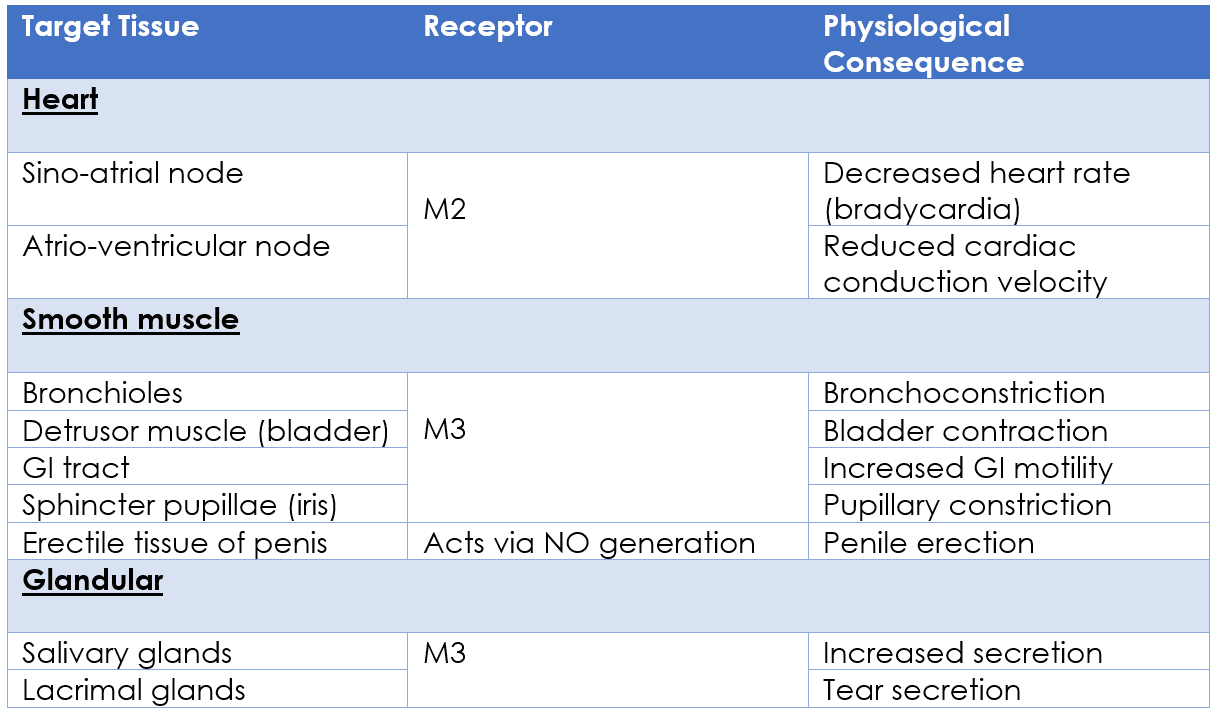
Table - The physiological actions of the parasympathetic nervous system
SimpleMed original by Dr. Joshua Bray
Role of Adrenaline in the Sympathetic Nervous System
As well as its neural component, the ‘fight or flight’ response also has an endocrine component: adrenaline.
Adrenaline is a tyrosine-derived hormone which is secreted into the bloodstream by chromaffin cells, located within the medulla of the adrenal glands. Chromaffin cells are essentially modified sympathetic post-ganglionic neurones which secrete adrenaline instead of noradrenaline.
Adrenaline acts on adrenoceptors in the same way that noradrenaline does, however because adrenaline is released into the bloodstream, it has a much more systemic effect (the ‘fight or flight’ response).
It is worth noting that some tissues have a much higher affinity for circulating adrenaline compared to noradrenaline - these tissues include bronchiolar smooth muscle and vascular smooth muscle of skeletal muscle arterioles.
For more information, check out our Endocrinology article on Adrenal Glands and Adrenal Disorders.
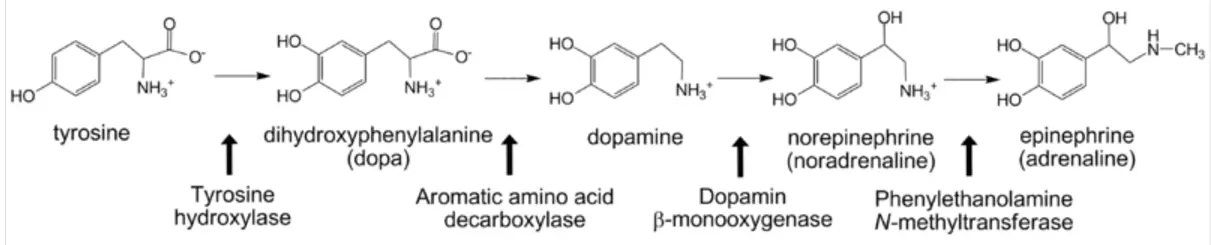
Diagram - Adrenaline biosynthesis from the amino acid, tyrosine
Creative commons source by Michael Skovbo Windahl [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)]
Drugs Affecting the Autonomic Nervous System
Drugs targeting the autonomic nervous system are often used to bring about a therapeutic effect. These drugs exert their effects by interacting with post-synaptic receptors or by interfering with neurotransmitter metabolism.
Common drugs targeting the SNS:
- Beta Agonists (e.g. salbutamol) - These drugs are used in the treatment of asthma as they cause bronchodilation via beta-2 adrenoceptor stimulation. However, as a side effect, beta agonists can cause tachycardia or palpitations due to interaction with beta-1 adrenoceptors in the heart; these side effects are greatly reduced due to the drug’s route of administration (inhalation).
- Beta Blockers (e.g. atenolol) - These drugs act by antagonising beta-1 adrenoceptors in the heart, resulting in reduced heart rate and contractility. They are therefore useful in the management of chronic heart failure, cardiac arrhythmias and hypertension, when used appropriately. A possible side effect of beta blockers is bronchoconstriction, due to interaction with beta-2 adrenoceptors in the lungs, and therefore care should be taken when prescribing this drug to asthmatic patients.
- Alpha Blockers (e.g. doxazosin) - These drugs cause smooth muscle relaxation by antagonising alpha-1 adrenoceptors. They are used in the treatment of benign prostatic hyperplasia and as an alternative therapy for hypertension. However, a common side effect of these drugs is postural hypotension due to interference with the baroreceptor reflex.
Common drugs targeting the PNS:
- Acetylcholine Esterase Inhibitors (e.g. donepezil) - These drugs enhance the effects of acetylcholine by inhibiting its breakdown by acetylcholinesterase (AChE). Donepezil is used in the treatment of Alzheimer’s disease and pyridostigmine is used in the treatment of myasthenia gravis (although this drug targets the neuromuscular junction, part of the somatic motor system). However, these drugs carry the risk of parasympathetic overload (SLUDGE syndrome) if the dose is too high.
- Muscarinic Agonists (e.g. pilocarpine, bethanechol) - Muscarinic agonists are rarely used in clinical practice due to a relative lack of selectivity and therefore a very high risk of systemic side effects (SLUDGE syndrome). However, there are some uses for these drugs when administered locally: pilocarpine eyedrops are used to treat glaucoma and bethanechol can be used under medical supervision to stimulate bladder emptying.
- Muscarinic Antagonists (e.g. atropine, tiotropium) - Atropine is used to reverse bradycardia as it antagonises the M2 receptors in the heart to increase heart rate. Inhaled antimuscarinics such as tiotropium are used to treat COPD and asthma as they cause bronchodilation via M3 receptor antagonism. A common side effect of antimuscarinics is a dry mouth, due to their inhibitory effect on saliva secretion.
Overstimulation of muscarinic acetylcholine receptors can lead to parasympathetic overload, otherwise known as SLUDGE syndrome, which can be life-threatening if not recognised and treated promptly. This is a medical emergency comprising the following symptoms:
- Salivation
- Lacrimation
- Urinary incontinence
- Defecation
- Gastrointestinal upset
- Emesis (vomiting)
Causes of SLUDGE syndrome include drug overdose (e.g. pyridostigmine), ingestion of ‘magic mushrooms’, exposure to organophosphorus insecticides or inhalation of nerve gas. Management includes intravenous antimuscarinics, such as atropine, alongside supportive care; additional agents may be required depending on the cause.
Reviewed by: Dr. Thomas Burnell
- 17051

