Next Lesson - Control of Plasma Volume
Abstract
- A single kidney contains between 800,000 - 1.5 million nephrons.
- The nephron can be split into multiple anatomical segments: glomerulus, bowman’s capsule, proximal convoluted tubule, loop of Henle, distal convoluted tubule, and collecting ducts - each segment differs in cell types and the role it plays.
Core
A nephron is the microscopic functional unit of a kidney - a single kidney can contain between 800,000 and 1.5 million nephrons on average!
There are two types of nephrons: cortical and medullary, named based on where in the kidney they are found. Both types of nephrons function very similarly, with small differences which will be discussed later.
This article aims to give an overview of the structure of the nephron - for more information on relevant ion and water transporters please see the article Control of Plasma Volume.
The nephron can be split up based on different cell types and their functions.
This diagram shows the difference between juxtamedullary nephrons (on the left of the image) and cortical nephrons (on the right of the image). Cortical nephrons are situated more peripherally in the kidneys, with the tip of the nephron descending just into the medulla. In contrast, the juxtamedullary nephrons have a longer Loop of Henle that extends deep into the renal medulla.
For more information on the structure of these nephrons and their individual blood supplies, please see our article on the Anatomy of the Urinary System.
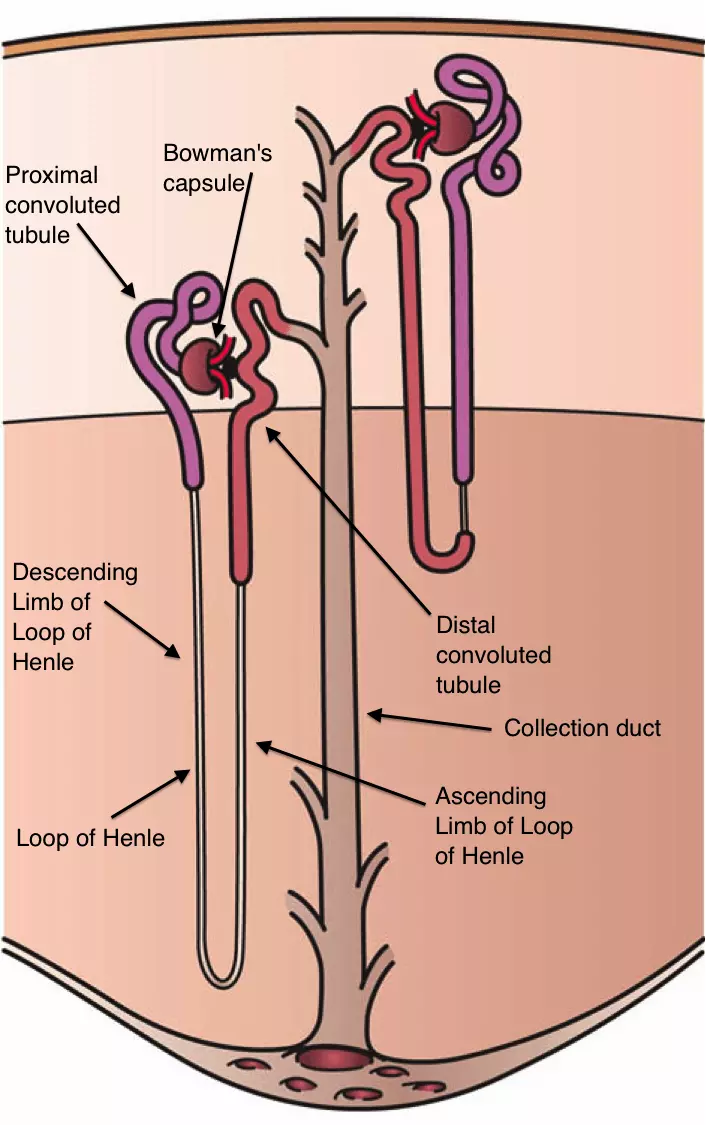
Diagram - An overview of a juxtamedullary nephron (left) and a cortical nephron (right)
Creative commons source by Holly Fischer [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)]
The glomerulus is a term that refers to the capillaries that exist between the afferent and efferent arterioles, and which are enclosed by the Bowman’s Capsule.
Blood flows through the glomerulus and is filtered - solutes and move into the Bowman’s capsule, flowing into the proximal convoluted tubule (PCT). Blood cells and proteins are not normally filtered, remaining behind in the vessels. The solution inside the PCT is referred to as the ultrafiltrate and different components of the ultrafiltrate are reabsorbed at different points of the nephron.
More information on the structure and function of the glomerulus can be found in our article on the glomerulus.
The PCT is responsible for reabsorbing many solutes including; sodium, chloride, potassium, bicarbonate, urea, amino acids, glucose, and water. Under normal physiological conditions, virtually all filtered amino acids and glucose are reabsorbed at the PCT.
The PCT is split into three segments, S1, S2, and S3 - based on the transporters which are expressed on the cell membranes.
The LoH is the part of the nephron which is responsible for setting up and maintaining the vertical osmotic gradient. This gradient is what allows solutes to be reabsorbed from the tubules. More information on the vertical osmotic gradient can be found in the article Control of Plasma Osmolarity.
The LoH can be split into the descending limb and ascending limb. The descending limb is permeable to water but impermeable to solutes like sodium, chloride, and potassium, whereas the ascending limb is impermeable to water but permeable to sodium, chloride, and potassium through the sodium-potassium-two-chloride (also known as NaKCl or NKCC2) transporter.
Distal Convoluted Tubule (DCT)
The DCT is responsible for reabsorbing sodium, chloride, potassium, calcium, magnesium, and bicarbonate. It is split into the early DCT (DCT1) and the late DCT (DCT2) - again based on the types of transporters expressed on the cell membranes.
The DCT is responsible for helping to maintain serum pH through the reabsorption of bicarbonate.
Thiazide and Amiloride diuretics act on transporters which are present in the DCT.
The CD is the last part of the nephron. It extends down into the renal medulla and eventually joins with other collecting ducts to form the renal calyces. They are responsible for the reabsorption of sodium, chloride, urea, and water from the ultrafiltrate.
The CD can be split into cortical and medullary segments based on their location. In the cortical CD there are two main cell types: principal cells which primarily reabsorb sodium, and intercalated cells which actively reabsorb chloride.
The reabsorption of water in the CDs can change in response to plasma osmolarity and is under the influence of antidiuretic hormone (ADH). The presence of ADH stimulates the insertion of aquaporin channels into the apical membrane of collecting duct cells - these channels allow water to pass through the membrane. This means that anti-diuretic hormone (as indicated by the name) encourages water reabsorption and therefore reduces the amount of urine produced.
The ultra-filtrate left after passing through the CD becomes urine. By this stage, the vast majority of filtered water has been reabsorbed, so what remains is a relatively small volume containing water, ions, metabolites, and nitrogenous waste.
All parts of the nephron have their own roles to play in the regulation of homeostasis. It is important to note that all the functions of all the parts of the nephron are happening simultaneously, and that the action of a drug or a hormone on one portion of the nephron causes an effect on the others.
Edited by: Dr. Maddie Swannack
Reviewed by: Dr. Thomas Burnell
- 7704

