Next Lesson - Anatomy and Physiology of the Midgut
Abstract
- The foregut is defined as the section of the gut from the mouth to the second part of the duodenum.
- It includes the mouth, oesophagus, stomach and first part of the duodenum. Developmentally, the liver, gallbladder, pancreas and spleen are also part of the foregut, but the anatomy and physiology of these structures are described in other articles.
- The foregut has ventral and dorsal mesentery.
- Its arterial blood supply is by the coeliac trunk, venous drainage is to the portal venous system (including via the splenic and left gastric veins), and it receives autonomic innervation from the vagus nerve with sympathetic fibres via the thoracic splanchnic nerves.
Core
The mouth is the first part of the gastrointestinal system (GI system), and it has two main functions (in relation to the GI system) - mechanical disruption of food by mastication and chemical disruption of food through digestive enzymes found in saliva.
The muscles involved in mastication are:
- Temporalis
- Masseter
- Medial pterygoid (jaw elevators)
- Lateral pterygoid (jaw depressor)
All the above muscles are innervated by the mandibular branch of the trigeminal nerve (CN V). For more information, please see our article Facial Planes, Muscles and Triangles (here) in our Head and Neck section.
Saliva is composed of water, potassium, bicarbonate, mucins, amylase, lingual lipase and immune proteins (such as IgA). These components of saliva work together to perform functions such as lubricating the oral cavity, maintaining oral hygiene and the initial chemical disruption of food.
Saliva is released into the oral cavity via three pairs of salivary glands: parotid, submandibular and sublingual (shown on the image below). Control of salivation is primarily driven by the autonomic nervous system.
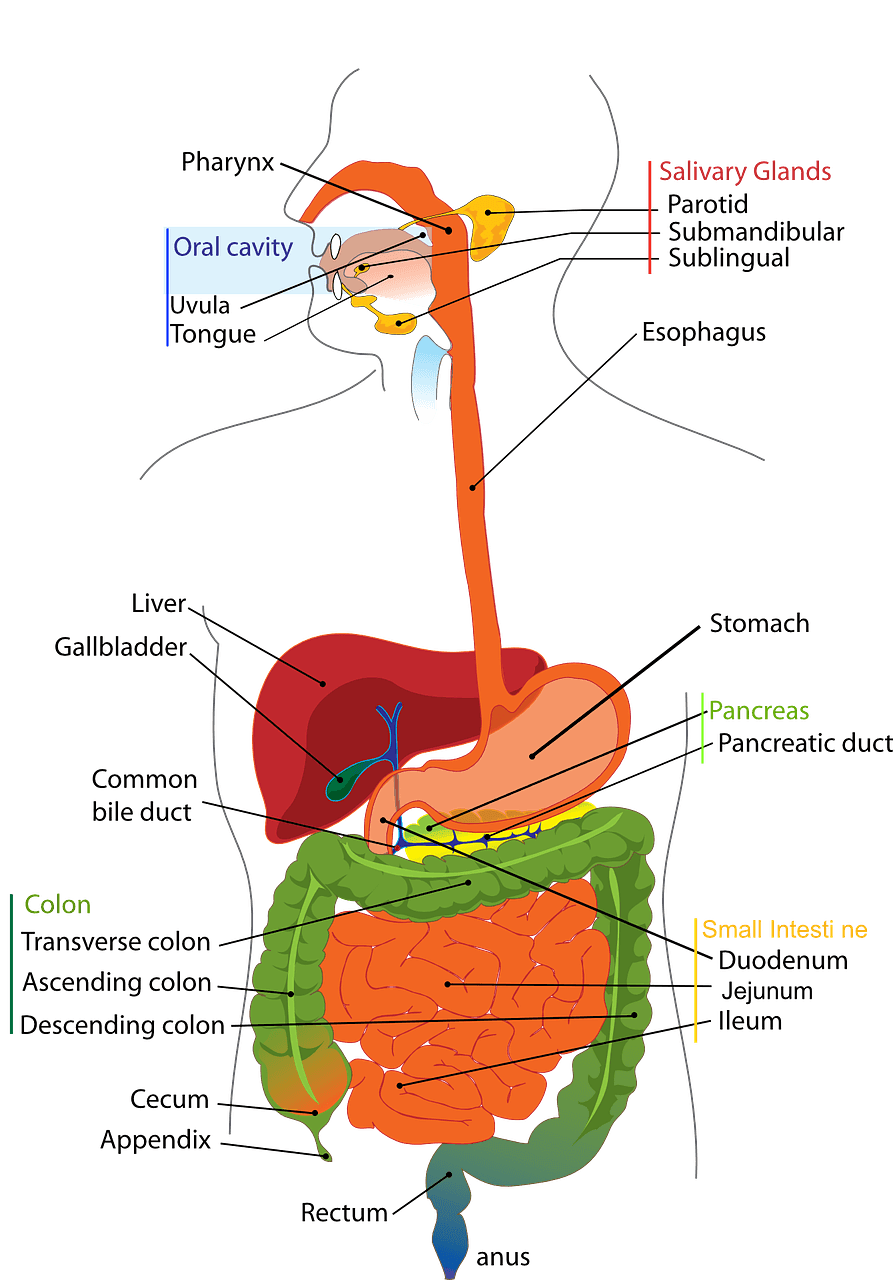
Diagram - Anatomy of the digestive system. The salivary glands are located in the head and all drain into the mouth
Creative commons source by Clker-Free-Vector-Images [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)]
The oesophagus is the muscular tube that allows food transportation from the mouth to the stomach. It sits posterior to the trachea in the neck.
The oesophagus undergoes rapid peristalsis in order to transport the food bolus from the mouth to the stomach. The upper oesophageal sphincter prevents air from entering the GI tract and the lower oesophageal sphincter prevents reflux of acidic stomach contents back into the oesophagus.
The stomach is the J-shaped organ that receives food from the oesophagus to further the digestion started by the mouth.
The stomach is anatomically divided into regions:
- Cardia - the cardia is the region that surrounds the lower oesophageal sphincter.
- Fundus - the fundus sits superior to the cardia; the stomach’s shape means there is a region superior to the lower oesophageal sphincter.
- Pylorus - the pylorus is the region at the bottom of the stomach, surrounding the pyloric sphincter which connects the stomach to the duodenum.
- Body - the body of the stomach is the largest portion of the stomach and makes up the region between the pylorus and the fundus.
The stomach’s unusual shape also means that its two edges have curves of different lengths. These are known as the greater curve of the stomach and the lesser curve of the stomach. They are shown in red on the diagram below.
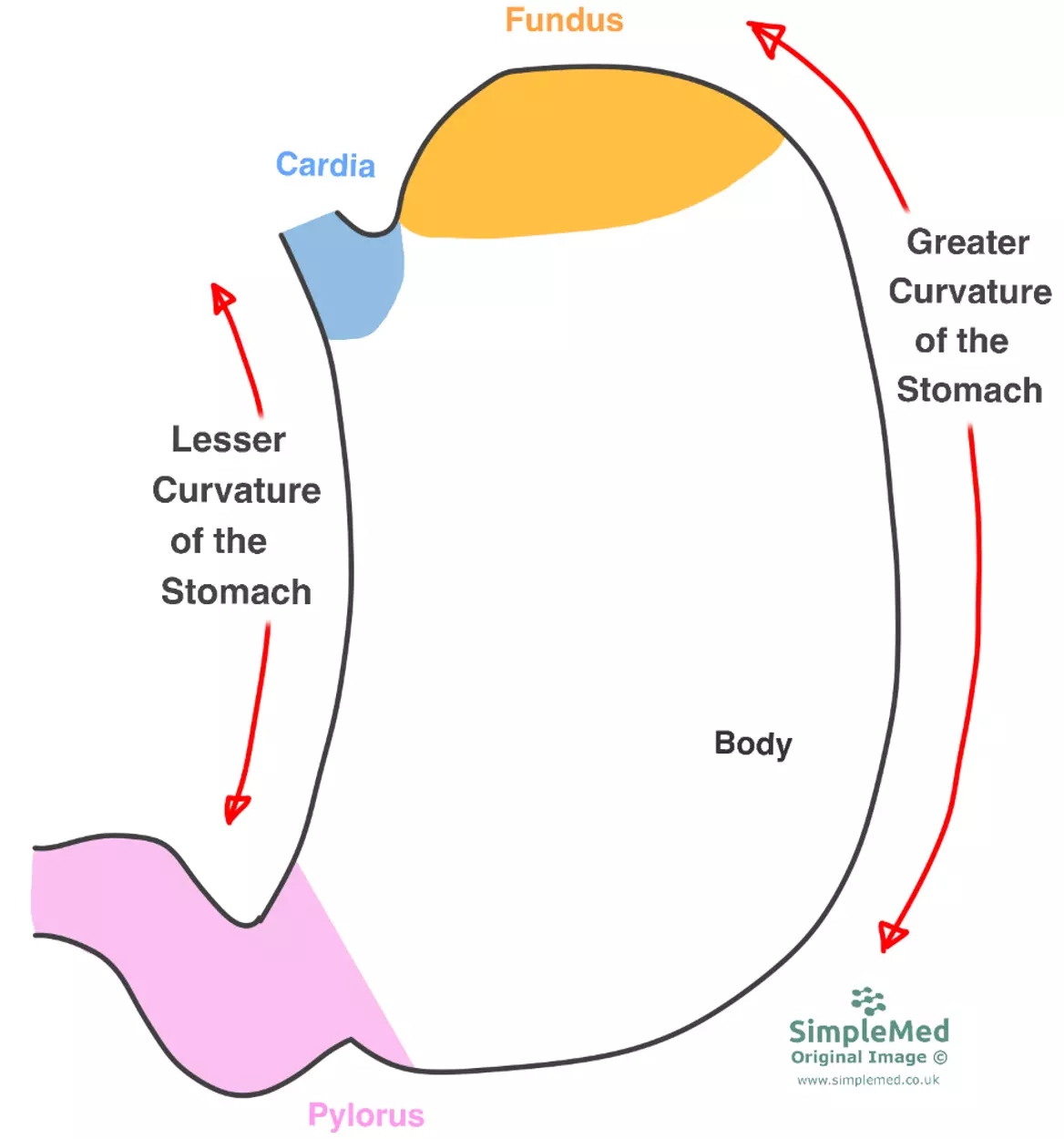
Diagram - The different regions of the stomach. Please note that the pyloric region of the stomach (shown in pink) is also known as the antrum
SimpleMed original by Dr. Maddie Swannack
The stomach also acts as an attachment point for the greater and lesser omenta. For more information on these, and the peritoneal cavity as a whole, please see our article Development of the Gastrointestinal Tract (here).
The stomach has three main functions:
- Storage of food
- Disruption of the food bolus to form chyme, through mechanical and chemical disruption
- Secretion of intrinsic factor
Mechanical disruption of the food bolus is aided by the stomach’s three layers of muscle that allow it to mix and grind its contents. These layers are the outer longitudinal layer, the central circular layer, and the inner oblique layer. By having fibres that run in three different directions, the stomach is able to contract against the food very well.
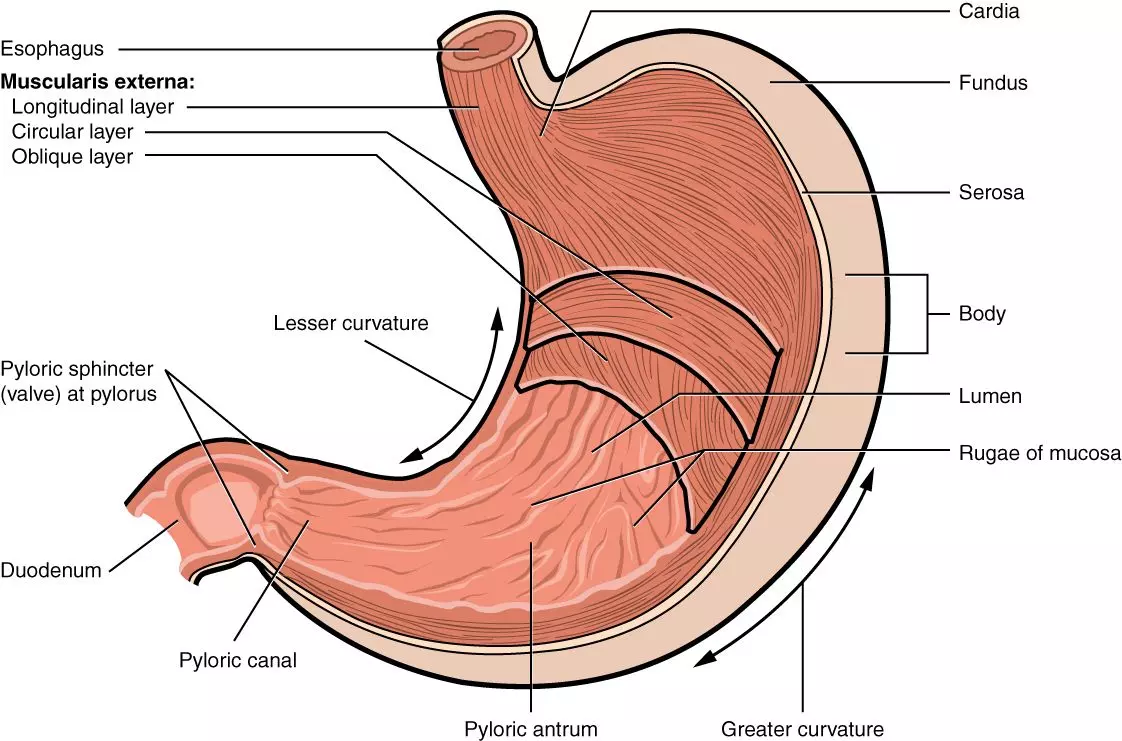
Diagram - Anatomy of the stomach with the three muscle layers shown
Creative commons source by OpenStax College [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)]
The stomach wall is lined by a mucosa that is ridged, meaning it can expand as food enters the stomach. These folds of mucosa are called rugae. This mucosa is an important part of the stomach, because it contains many specialised cells that assist with digestion that are arranged in gastric pits, specialised folds of epithelium that act to increase surface area.
G Cells - These are found within the pylorus. They are stimulated by gastrin-releasing peptide (GRP), acetylcholine release from neurones, and the presence of amino acids in the stomach to secrete gastrin to increase gastric acid secretion.
Parietal Cells - These are found within the body and fundus. They are stimulated by gastrin to secrete HCl to digest proteins, activate proteases and disinfect stomach contents. They also release intrinsic factor to aid Vitamin B12 absorption in the terminal ileum.
Mucous Cells - These are found within the cardia, body and fundus. They secrete mucus and HCO3- ions to form a thick alkaline layer that adheres to the epithelium of the stomach to protect it from acidic damage.
Chief Cells - These are found within the fundus and body. They secrete pepsinogen to chemically disrupt proteins.
D Cells - These are found within the pylorus. They are stimulated by the pH decreasing to secrete somatostatin to inhibit G cells. This fall in pH occurs when the digested food leaves the stomach, meaning any acid secretion that continues is not buffered by the food.
As well as mucus and HCO3- ion secretion, the stomach has other defences including a high turnover of epithelial cells and an increased blood flow to the mucosa which is maintained by prostaglandins.
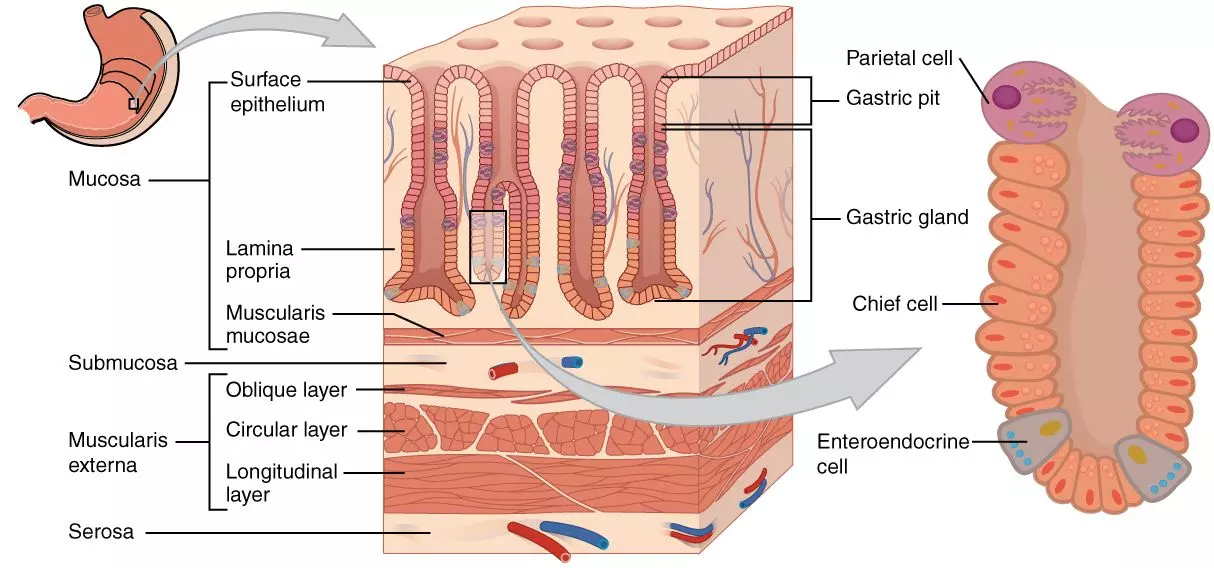
Diagram - Histology of the stomach with the cells found within the gastric pits
Creative commons source by OpenStax College [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)]
The duodenum is the most proximal part of the small intestine. It is the section of the gut between the pylorus of the stomach and the start of the jejunum, and it is split into 4 parts.
The function of the duodenum is to neutralise the acidic chyme from the stomach with HCO3- rich secretion before it enters the jejunum. This is achieved mainly through bicarbonate-rich pancreatic secretions released into the duodenum, with bile contributing to digestion of fats. It is also where iron is absorbed from the chyme.
The duodenum has a dual blood supply from the gastroduodenal artery (a branch of the coeliac trunk) and the inferior pancreaticoduodenal artery (a branch of the superior mesenteric artery). Its venous drainage is into the veins of the same name, which then drain directly into the portal vein. Lymphatic drainage is into the pancreatoduodenal and superior mesenteric nodes.
I Cells - stimulated by the presence of fats and proteins, I cells release cholecystokinin (CCK) to increase pancreatic and gallbladder secretions.
S Cells - stimulated by H+ and fatty acids to secrete secretin. This increases HCO3- secretion and decreases gastric acid secretion from the stomach.
K Cells - stimulated by sugars, fatty acids and amino acids to secrete gastric inhibitory polypeptide (GIP). This acts to increase insulin secretion and decrease gastric acid secretion.
Edited by: Dr. Maddie Swannack
Reviewed by: Dr. Thomas Burnell
- 8843

