Next Lesson - The Postpartum Period
Abstract
- Labour can be divided into three stages, each with specific beginning and end points.
- The first stage is from onset of labour to 10cm cervical dilation. The second stage is from 10cm dilation of the cervix to delivery of the baby. The third stage is from delivery of the baby to delivery of the placenta and membranes.
- Prostaglandins play an important role in initiating labour and can stimulate uterine contractions along with oxytocin.
- Before it can dilate, the cervix ‘ripens’, and effaces (thins).
- The muscle fibres in the uterus are specialised to contract, then not fully relax (called retraction), allowing the progressive shortening of the fibres. The contractions are brought on by Ca2+ release, stimulated by prostaglandins and oxytocin.
- Through vaginal delivery the baby undergoes a number of movements: flexion, internal rotation, crowning, extension, restitution, rotation, and delivery.
- With fetal or maternal distress interventions like assisted vaginal delivery (through Ventouse or Forceps) or Caesarean section can be considered.
- Fetal distress can be detected with CTG monitoring (non-invasive) or fetal blood sampling (invasive).
- The diameter of the birth canal, the power and frequency of contraction, and features of the fetus can all affect labour. The lie, presentation, position, degree of neck flexion, and moulding of the fetal skull can all either help or hinder labour.
- The third stage of labour is the delivery of the placenta, and can be actively managed with oxytocin to help avoid post-partum haemorrhage.
Core
Labour is defined as the physiological process by which a fetus is expelled from the uterus to the outside world.
Delivery is the method of expulsion of the fetus, thereby transforming the fetus into a neonate.
Gravidity is a characteristic of the mother describing the total number of pregnancies this woman has had. This includes the current pregnancy and any previous pregnancies, including miscarriages, stillbirths and terminations.
Parity is another characteristic of the mother describing the total number of births she has delivered with the fetus after 24 weeks of gestation. If the mother is still pregnant, it does not include the current pregnancy (because she has not given birth yet). It therefore includes any previous children, stillbirths or late-term terminations (such as for medical reasons).
Overall, labour involves changes to the cervix followed by co-ordinated changes to the uterine myometrium. The whole process aims to achieve two things: dilate the cervix so the fetus can pass through and push the fetus through the birth canal.
The first stage of labour aims to create the birth canal. It is clinically defined as the interval between the onset of labour and full (10cm) dilation of the cervix.
The birth canal is made up of the pelvic bones, the lower uterine segment, the cervix, the vagina, the vulva, the pelvic floor, and the perineum - these can collectively be referred to as ‘the passage’.
Through this process, the birth canal is created and the fetus’ head descends into it.
There are two phases of the first stage of labour; the latent phase and the active phase.
The latent phase describes the onset of labour with slow cervical dilation and cervical softening. This can last for a variable amount of time depending on the parity of the mother, with multiparous women generally having a shorter latent first stage, and a shorter overall labour.
The latent phase progresses into the active phase where there is a faster rate of change to the cervix and regular uterine contractions aiming to further dilate the cervix.
The second stage of labour is the time between full dilation of the cervix and delivery of the fetus. The uterine contractions change to become expulsive, which leads to the descent of the fetus through the birth canal through to delivery. The second stage involves passive elements (descent of the fetus and rotation of the fetal head, reducing the circumference of the fetal head in relation to the birth canal), and active elements (maternal effort to expel the fetus and achieve birth - pushing).
The third stage of labour starts when the baby is birthed and ends with the complete expulsion of the placenta and the membranes. The uterus achieves this through further contractions. This usually lasts between 5 and 15 minutes, but can last up to an hour depending on the clinical circumstances.
First Stage of Labour: Initiating Labour
In order to start labour, the myometrium becomes progressively more excitable, through increased gap junction communication between smooth muscle cells, and the cervix begins to ripen. The exact mechanism behind this is unknown, but it is known that prostaglandins play an important role, which is why they can be used to initiate labour in women who are overdue to give birth.
Prostaglandins are biologically active lipids which act as local hormones and are produced by the myometrium and the decidua (the endometrium which has been modified for labour). The production of prostaglandins is controlled by the oestrogen:progesterone ratio, with higher levels of oestrogen promoting prostaglandin release.
Rising levels of prostaglandins stimulate powerful contraction of the smooth muscle and cervical softening. The cervical softening is also helped by oestrogen and the hormone relaxin, which work in combination with prostaglandins to break down the connective tissue. Progesterone inhibits contractions.
Oxytocin is a hormone which stimulates and augments uterine contractions. It is secreted from the posterior pituitary gland under control of the hypothalamus. Its action is inhibited by high levels of progesterone, relaxin, and low number of oxytocin receptors in the myometrium.
At 36 weeks of pregnancy, there is an increased number of oxytocin receptors present in the myometrium, meaning the uterus is better able to respond to pulses of oxytocin released from the posterior pituitary.
Oxytocin stimulates the uterus to contract, and also stimulates the placenta to synthesise prostaglandins, which then go on to stimulate more contractions of the uterus. Uterine contractions have a positive feedback effect on oxytocin release and prostaglandin synthesis.
During pregnancy, the cervix is responsible for retaining the developing fetus. A cervix which cannot do this is termed incompetent and can result in miscarriage. For this reason, the cervix is tough, thick, and high in collagen. Whilst this is good for pregnancy, the cervix needs to soften before labour can begin. This process is called cervical ripening.
Cervical ripening involves reducing the amount of collagen, increasing the amount of glycosaminoglycans, and increasing the amount of hyaluronic acid in the extracellular matrix of the cervix. This causes reduced aggregation of the collagen fibres which makes the cervix softer. This process is triggered by prostaglandins PGE2 and PGF2α. Cervical ripening is also stimulated through increasing levels of relaxin during pregnancy.
Overall, due to cervical ripening, the cervix offers less resistance to the presenting part of the fetus.
The cervix is said to be effaced and dilated at the time of delivery.
Effacement is the thinning of the cervix through the opening of the internal cervical os (but the external cervical os is still closed).
Dilation is the separation of the external cervical os to allow the birth of the baby.
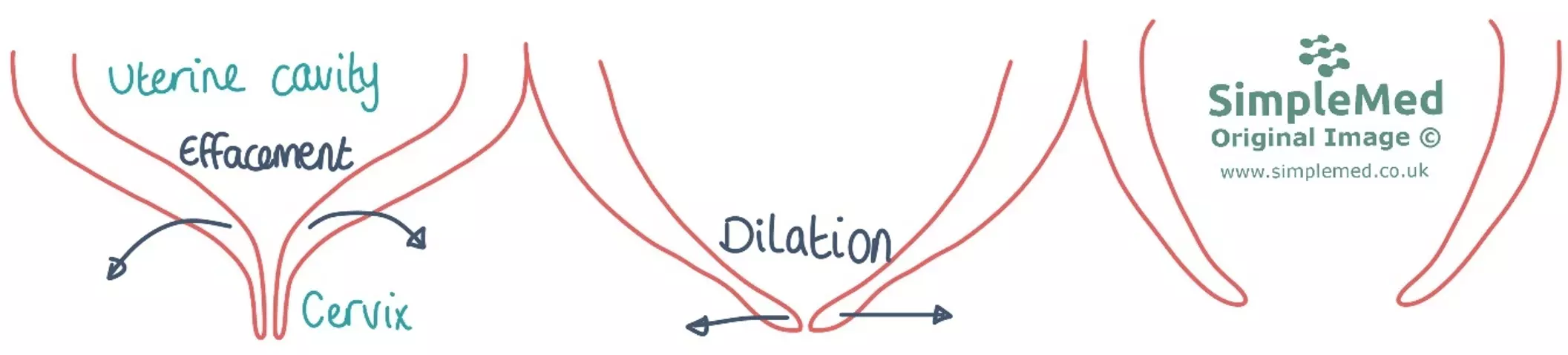
Diagram - The difference between effacement and dilation of the cervix in labour
SimpleMed original by Dr. Maddie Swannack
Artificial Induction of Labour
There are a number of methods clinicians use to initiate labour, each with their own specific indications depending on what the clinician thinks the problem may be. We can stimulate the release of prostaglandins through an Artificial Rupture of the Membranes (ARM). Artificial prostaglandins are another option, and these can be given orally or vaginally. Another effective method of inducing labour is intravenous synthetic oxytocin (Syntocinon), however, if this is being used there must be continuous fetal monitoring and more regular maternal observations. Finally, anti-progesterone agents can also be used to induce labour.
First Stage of Labour: Uterine Smooth Muscle Physiology
The myometrium has specific adaptations compared to normal smooth muscle, to help facilitate labour and delivery. A normal muscle contracts and relaxes. The myometrium contracts like any other muscle, but only partially relaxes which causes permanent shortening of the muscle fibres. This process is called contraction and retraction. It helps to expel the fetus through the birth canal, because the uterine cavity becomes progressively smaller.
Contractions start in the two poles of the uterus (the upper parts of the uterus near the entrance of the fallopian tubes). The contractions spread to the uterine fundus and upper segment of the uterus, before moving down to the lower segment. The contractions in the upper segment are more powerful than those in the lower segment.
The contraction force of the myometrium is generated when intracellular concentrations of Ca2+ ions increase following membrane depolarisation and action potential activity. Contractions are made more forceful and frequent by prostaglandins and oxytocin, which promote calcium entry and release and increase uterine muscle excitability.
The Second Stage of Labour: Normal Process of Vaginal Delivery
During the second stage of labour, the fetus undergoes a series of movements in order to help it deliver:
- Head Flexion - the fetal head flexes as the diameter of the occipital portion of the head is smaller than the top of the head
- Head Internal Rotation
- Crowning - the head stretches the perineal muscle and skin
- Extension of Head and Restitution - after the head is crowned the head extends and externally rotates to allow for delivery of the shoulders
- Rotation and Delivery of the Shoulders
- Delivery of the Rest of the Body - this happens rapidly after the head and shoulders are delivered
The second stage of labour is a high risk part of labour. Both the mother and the fetus are monitored closely to ensure the second stage is progressing well. If there are signs of fetal or maternal distress, there are a number of options to help deliver the fetus.
An operative delivery is an assisted vaginal delivery. This can be done using forceps on the fetus’ head or through vacuum extraction by placing a suction cup (Ventouse machine) on the fetus’ head. These are not without risk as they can cause damage to the baby, but it is often used with evidence of fetal distress so is the best choice overall.
A caesarean section can be done electively (planned), in an emergency, or when an operative delivery has failed. An incision is made in the skin and the uterus and the fetus is delivered through the incision. This has some advantages in that it can be done quickly in an emergency with a well-trained and well coordinated team. But it has some risks similar to any other major surgery such as infection, bleeding, damage to nearby structures (bowel and bladder in particular), scar formation, and iatrogenic damage to the fetus.
Monitoring of the Fetus During Labour
Monitoring the fetus is like monitoring observations on any other patient, but in fetuses it must be done indirectly.
One of the most popular methods of measuring fetal wellbeing is the cardiotocograph (CTG). A CTG is essentially a belt which is placed on the mother’s abdomen and contains two sensors to measure fetal heart rate and the frequency and duration of uterine contractions. This is a non-invasive method of measuring fetal wellbeing and the results are printed out on a graph to allow for observation over a long period of time.
Other methods of monitoring fetal wellbeing are looking at mother’s temperature, looking at the colour and amount of amniotic fluid being produced, or by making a very small cut on the fetal head and measuring the capillary pH - this is called fetal blood sampling (FBS).
The Three Ps: Problems with Labour
There are three Ps that describe things that can affect delivery of a fetus.
In a normal vaginal delivery, the fetal head is the biggest part, measuring around 9.5cm in diameter. The pelvic inlet usually measures around 11cm, although the softening of ligaments may increase this slightly. This means that there isn’t a lot of difference between the size of the fetal head and the pelvic inlet, meaning a number of mechanisms are needed to help the fetus be delivered. One of these mechanisms is the stretching of the fibres of levator ani (a pelvic floor muscle) and the thinning of the central portion of the perineum.
If the passage does not increase in size, or if the maternal pelvis is abnormal, normal vaginal delivery can be very difficult.
The frequency of contraction of the myometrium and the power of the contractions contribute to the possibility of normal vaginal delivery. In the first stage of labour, the contractions should ideally be every 3-4 minutes. In the second stage of labour, the contractions should ideally be every 2-3 minutes.
If the contractions are not happening quickly enough, an IV infusion of oxytocin can be given. If the contractions are happening too quickly (this is common if the oxytocin infusion has been given), a different drip can be given to slow contractions, a process called tocolysis.
The position of the fetus can also affect labour.
Lie: The lie of the fetus describes the orientation of the long axis of the fetus (head to feet) in comparison to the long axis of the mother. It can be long (head down), oblique (head towards the pelvic bone), or transverse (head to the side). Only long lie babies can be delivered vaginally.
Presentation: The lowest part of the fetus, the part that will come out of the vagina first. The possibilities are cephalic (head first), breech (bottom first), or shoulder presentation. Cephalic is the best presentation for vaginal birth. Breech vaginal delivery is possible but rarer. Shoulder presentation should not be attempted vaginally.
Position: The description of which way the baby is orientated within the presentation. For example, for cephalic presentation, this is which way the baby is looking, or with breech presentation, this is the direction of the sacrum.
- Occipitoanterior - baby is looking at the mother’s spine, their occipital bone is anterior.
- Right Occipitotransverse - baby is looking to the mother’s left side, with the occipital bone towards the maternal right thigh.
- Left Occipitotransverse - baby is looking to the mother’s right side, with the occipital bone towards the maternal left thigh.
- Occipitoposterior - baby is looking out the front, ‘back to back’.
Occipitoanterior is the easiest position to deliver the baby vaginally, but all are possible. Babies that are occipitotransverse often rotate to allow easier delivery of the shoulders.
Flexion: As described earlier, when the fetus is being born, it undergoes a number of movements, one of which is neck flexion. The degree of neck flexion is important, because increased flexion decreases the diameter of the head and so encourages easier vaginal birth.
The position that is ideal for delivery is occipitoanterior with lots of neck flexion (chin on chest), as this creates the smallest head diameter. If the neck is not flexed this much, or in the occipitoposterior position, the diameter is larger and this can slow the first or second stages of labour.
Moulding: The sutures in the fetal skull also allow for moulding, when the suture lines overlap and shuffle to allow the circumference of the head to decrease. This means that babies just after vaginal birth may not have a normal shaped head.
After the baby is born, there is a massive reduction in the size of the uterus, but the contractions continue. This causes squeezing of the placenta which causes it to separate from the uterus and descend.
There are a number of mechanisms which act to reduce the amount of blood lost after the delivery of the placenta; the failure of any of these mechanisms can lead to a postpartum haemorrhage.
The powerful contraction and retraction of the uterus continues after delivery of the placenta, and cuts off the blood vessels that supplied the placenta.
The third stage can be ‘actively managed’, which involves an intramuscular injection of oxytocin given into the thigh. This encourages uterine contraction, which decreases the chance of post-partum haemorrhage. This is not essential, and some women opt to not have the injection.
For information on changes that occur to the fetal circulation after birth, see the article here.
Edited by: Dr. Maddie Swannack
Reviewed by: Dr. Thomas Burnell
- 3758

