Next Lesson - Behaviour of Neoplasms
Next article - Behaviour of Neoplasms
Abstract
- Carcinogenesis is the process by which neoplasms develop and classically involves initiation, promotion and progression.
- This occurs due to a combination of intrinsic factors such as age, and germline mutations, and extrinsic factors such as behavioural factors and carcinogen exposure.
- Tumour suppressor genes normally inhibit growth of tumours. Enhanced tumour growth requires two mutations of these genes - one to each allele.
- When a proto-oncogene is mutated it becomes an oncogene, which enhances growth of tumours. Only one of these alleles needs to be mutated to allow tumour growth.
- There are several recognised hallmarks of cancer. A key distinction is that only malignant neoplasms have the ability to invade surrounding tissues and produce metastases.
Core
Cancers are formed by the accumulation of DNA mutations in cells that allows them to proliferate out of control. The risk of cancer growth is accounted for by a combination of intrinsic host factors (e.g. age, gender) and extrinsic factors relating to environment and behaviour.
4 in 10 UK cancer cases can be prevented by lifestyle changes*. The main modifiable risk factor for cancer is smoking, and others include obesity, alcohol, an unhealthy diet and lack of physical activity. It’s important that patients are made aware of this so they can make necessary changes to their lifestyle to reduce their cancer risk. Some behavioural factors are also classed as carcinogens such as smoking.
A carcinogen is an environmental agent which can cause cancer through mutation of DNA, some of which are avoidable and others cannot be avoided. Carcinogens can be identified from:
- Epidemiological studies (looking at carcinogen exposure in the population).
- Testing on laboratory animals or bacteria.
Carcinogenic agents can include chemicals, radiation or infection.
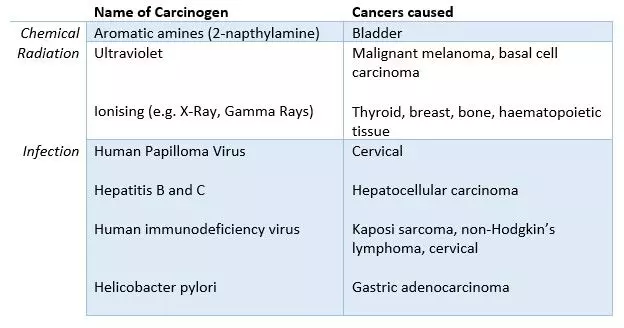
Table - Carcinogens and the types of cancer they commonly cause
SimpleMed Original by Dr. Emily Smith
Carcinogens can also be further split into either initiators or promoters. An initiator carcinogen starts the process by mutating the cell DNA, and for a neoplasm to develop, exposure to initiator carcinogens is typically required initially, but other factors may also contribute. Exposure to a promoter carcinogen then causes prolonged proliferation. This allows for expansion of mutated monoclonal cells to form a neoplasm. Through the process of progression (talked about later), this collection of cells becomes a malignant mass.
Occupational Exposure to Carcinogens
Asbestos
This is a substance which was commonly used in the building and construction industries. Asbestos fibres can be released into the air and breathed in, resulting in inflammation and scarring of the lungs. Exposure to asbestos is associated with several different types of cancer including mesothelioma - cancer of the pleura. People who are at risk of this are those whose jobs involve regular exposure to asbestos, such as demolition workers, asbestos removal workers and firefighters.
Dye Industry
2-naphthylamine was a chemical used in the dye manufacturing industry. However, it was later found to be a carcinogen which causes bladder cancer, so is now no longer used.
The identification of occupational carcinogens allowed several points to be understood about the contribution of carcinogens to the development of cancer:
- Often there is a long delay between carcinogen exposure and development of a malignant neoplasm.
- There can be organ specificity for carcinogens.
- The risk of cancer development increases with total dosage of the carcinogen.
The risk of developing cancer is also influenced by several important host factors. These include:
- Skin pigmentation - Increased melanin in the skin reduces the risk of skin cancer as it blocks ultraviolet light.
- Sex - Breast cancer is more likely in women due to a greater amount of breast tissue and endocrine factors.
- Age - Cancer incidence increases with age due to many factors, including the accumulation of mutations and loss of protective factors.
- Medical conditions - Cirrhosis is associated with hepatocellular carcinoma, and ulcerative colitis is associated with colorectal cancer due to prolonged injury and inflammation to the organs.
- Inherited risks - Due to germline mutations.
A germline mutation is a detectable variation within the DNA of germ cells (sperm and ova), which can therefore be passed on to offspring. These include mutations to tumour suppressor genes, proto-oncogenes or genes which control DNA repair. If a person has a germline mutation, they are much more likely to develop a neoplasm during their life. This is why some cancers run in families - because their genes make them more susceptible, and these genes are passed down through the generations.
Tumour Suppressor Genes
Tumour suppressor genes normally inhibit growth of tumours. Both alleles of this gene (one on each chromosome) need to be inactivated to allow growth of tumours.
- Retinoblastoma (Rb gene)
- Normally the Rb gene stops damaged cells from passing the restriction point in the cell cycle, preventing the cell from replicating.
- Inactivation of both alleles therefore allows uncontrolled movement through this point, allowing cells to divide.
- This germline mutation results in familial retinoblastoma, and children with the faulty gene can develop this cancer at a very young age.
- p53 gene
- Normally encodes for a transcription factor involved in repairing DNA.
- Repairs damage in the S phase of the cell cycle or causes apoptotic cell death if the damage is too extensive.
- Inherited mutations result in Li-Fraumeni syndrome, which increases the risk of developing several cancers including osteosarcoma, breast cancer, melanoma and many more.
The two-hit hypothesis demonstrates how a person with a germline mutation of a tumour suppressor gene on one chromosome is more likely to develop a neoplasm. If one tumour suppressor gene is inherited as mutated - the “first hit” - then the second gene can still protect the cell to suppress tumour growth. However, if the second gene becomes mutated and the cell is no longer protected - the “second hit” - then the chance of tumour growth is very high.
A person with no germline mutation is much less likely to develop a neoplasm as they require both “hits” which is unlikely.
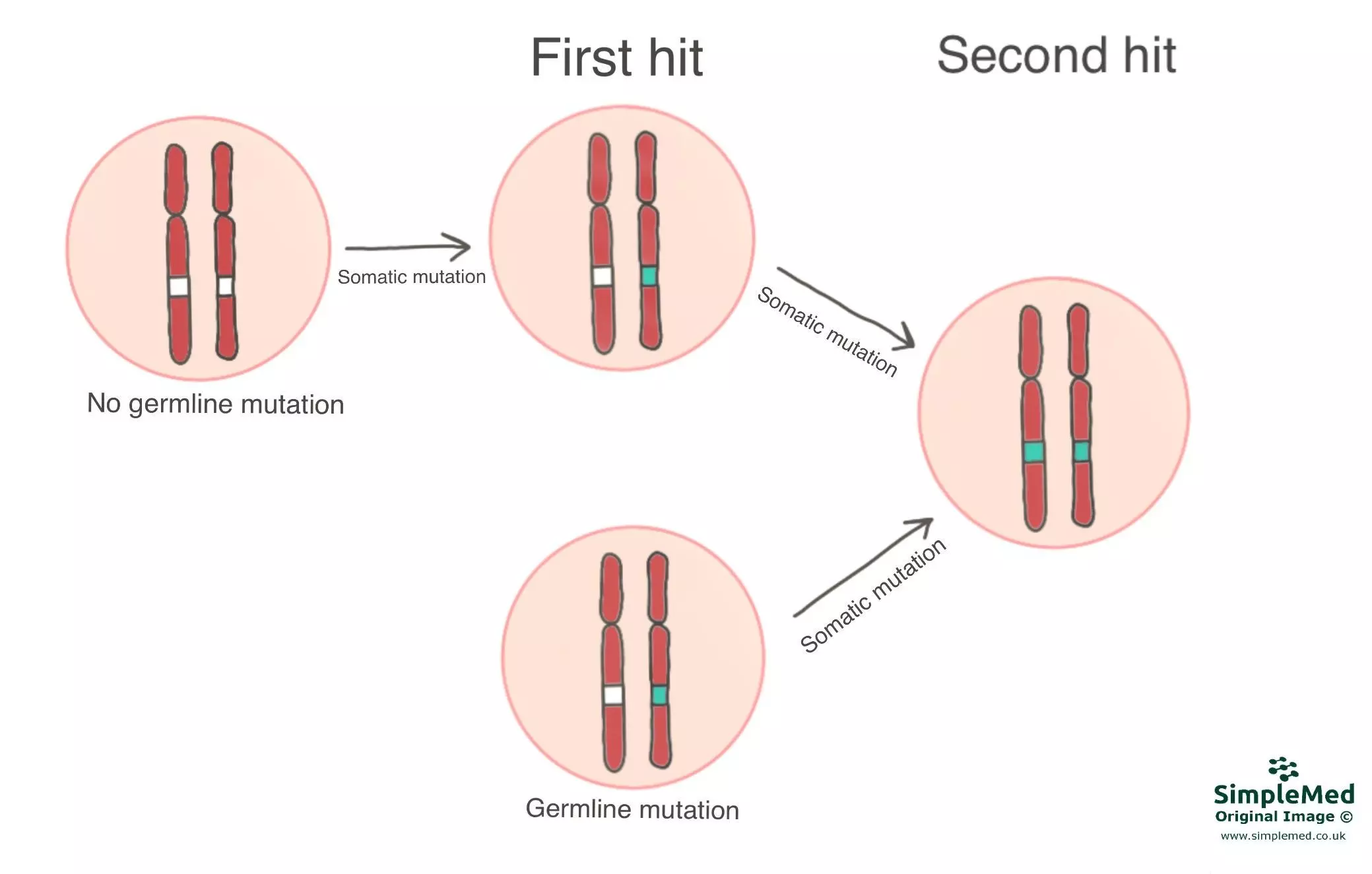
Diagram - A demonstration of the "two-hit" hypothesis of gene mutations leading to cancer
SimpleMed Original by Dr. Emily Smith
Proto-Oncogenes
When a proto-oncogene is mutated it becomes an oncogene. A mutation of this gene enhances growth of tumours. Only one of these alleles needs to be mutated to allow growth of tumours because you can add functions with only one mutation.
- RAS
- Codes for a G protein which signals for a cell to get past the restriction point in the cell cycle.
- A mutation causes this protein to always be active, and therefore the cell constantly moves through the cell cycle and divides.
- HER-2
- Codes for growth factor receptors.
- Overexpression of this gene leads to many growth factor receptors being expressed on the tumour cell surface, increasing the sensitivity of the cell to growth factors.
- This accelerates growth of the neoplasm, and is particularly associated with breast cancer.
DNA Repair Genes
DNA repair can be affected in several different ways by germline mutations, and therefore can result in inherited clinical syndromes.
- Individuals with xeroderma pigmentosa have reduced ability to repair UV damage, and therefore they are more likely to develop skin cancer at a young age.
- Familial breast carcinoma is associated with mutations to the BRCA1 or BRCA2 genes, which are normally involved in repairing double strand DNA breaks.
- Hereditary non-polyposis colon cancer (HNPCC) is a condition affecting DNA mismatch repair genes, which increases the risk of developing colorectal cancer.
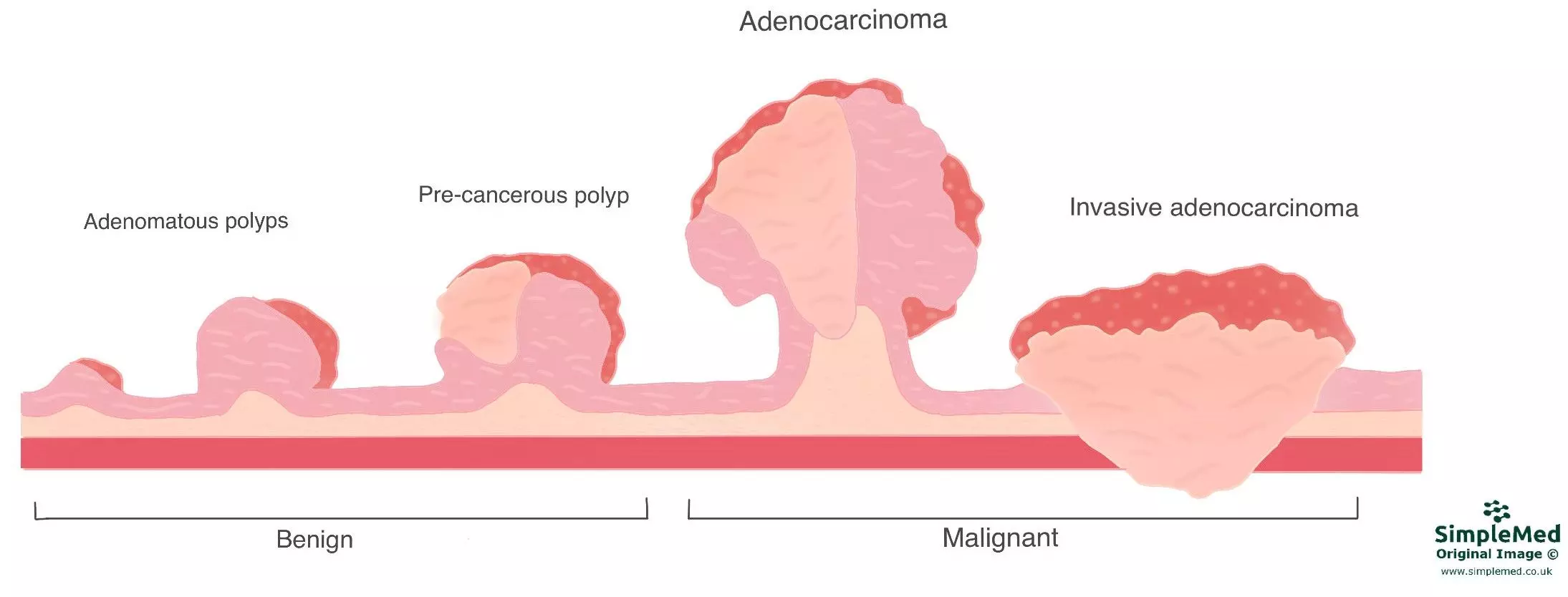
Diagram - Demonstrates the progression from a benign polyp in a glandular area of the body to an invasive malignant adenocarcinoma
SimpleMed Original by Dr. Emily Smith
There are six hallmarks of cancer classically described in fully evolved malignant neoplasms, although this framework has since been expanded. These characteristics are due to mutations of the DNA of the cancer cells.
- Self-sufficiency in growth signals
- Resistance to growth stop signals
- Cell immortalisation through the action of telomerase
- Angiogenesis; the ability to produce new blood vessels
- Resistance to apoptosis
- Ability to invade and produce metastases
The first five of the above features can apply to both benign and malignant neoplasms, whereas the sixth is specific to malignant neoplasms.
Genetic instability is an enabling characteristic of the development of neoplasms rather than a hallmark.
Edited by: Dr. Bethany Turner
Reviewed by: Dr. Maddie Swannack
*Source: Cancer research UK, cancer statistics for the UK - https://www.cancerresearchuk.org/health-professional/cancer-statistics-for-the-uk date accessed: Dec 2019
- 13013

